This publication is produced in partnership with Project UNITY’s Catalyst Academy Class of 2025, a student public health research and education program.

Abstract
Childhood obesity is a growing public health issue in the United States, with exceptionally high rates among low-income and minority communities. In Houston, Texas, the condition is particularly prevalent, as many families face barriers to nutritious food and affordable healthcare. Low-income communities are often the most affected, as financial limitations directly affect families’ access to healthy and affordable food options, increasing children’s risk of obesity. Addressing this issue through a public health lens allows for a deeper focus on prevention and long-term health outcomes. The purpose of this report is to examine the impact of childhood obesity on low-income communities in Houston, identify key social determinants that drive the issue, and design a community-based intervention to address those factors. We conducted research using peer-reviewed sources such as PubMed and Google Scholar, reviewing 20 scholarly articles on prevention strategies, social determinants of health, and successful intervention models. Articles were selected based on relevance, credibility, and frequency of citation in public health research. Findings show that Hispanic and Latino children living in low-income Houston neighborhoods are at the highest risk for obesity, with the main contributing factors including food insecurity, limited access to safe recreational spaces, inadequate healthcare access, and lower educational and economic opportunities. While programs like Coordinated Approach To Child Health (CATCH) and CAN DO Houston have made significant progress, gaps in awareness and accessibility remain. This report proposes a combined intervention method that integrates digital solutions, with a focus on nutritional education resources and culturally relevant support. In the long term, the goal is to scale this model to other underserved communities across the nation.
Keywords: Childhood obesity; socio-economic determinants; nutrition; lifestyle; diet; public health intervention
Introduction
Childhood obesity is a medical condition that occurs when a child is significantly overweight for their age and height, as measured by Body Mass Index (BMI) percentiles. It is defined as having a BMI at or above the 95th percentile for children of the same age and sex (Sanyaolu et al., 2019). In recent decades, childhood obesity has become one of the most pressing public health concerns in the United States, with 1 in 5 children classified as obese (CDC, 2024). If left unaddressed, it can lead to serious health, social, and financial strain. Health-wise, it increases the risk of chronic conditions like Type 2 diabetes, high blood pressure, joint problems, and mental health issues such as anxiety and low self-esteem (Sanyaolu et al., 2019). Social consequences include bullying, teasing, and social exclusion due to their weight, leading to isolation, low self-confidence, and shorter interaction with peers. These social stressors can create a cycle that discourages physical activity, worsening physical and mental health outcomes. Financially, childhood obesity places a burden on families through additional doctor visits, medication, and therapy (Sanyaolu et al., 2019). If not appropriately treated, children with obesity are more likely to experience obesity in adulthood, contributing to long-term healthcare costs. The objective of this report is to investigate childhood obesity at both national and local levels, identify the main social determinants contributing to the rising rates of obesity among children from low socioeconomic backgrounds, and design an evidence-based intervention to promote healthier lifestyles and reduce obesity related risks.
The report highlights the public health significance of childhood obesity within the socioeconomic model. We examine relevant literature, explain the target population selection process, and present findings from a stakeholder with experience in childhood obesity research. Using a comprehensive framework that addresses prevention and accessibility, this research proposes a 12-month plan to improve healthy practices and reduce obesity rates among youth/children. Strengths and limitations of the proposed intervention and how we can improve its impact are also discussed.
The Importance of a Public Health Lens
Addressing childhood obesity through a public health lens is essential, especially in communities such as Houston, Texas, where this health issue disproportionately affects low-income families (Salahuddin et al., 2017). Clinical intervention focuses on the individual, whereas public health intervention targets social and environmental determinants and aims to prevent. A public health intervention helps support fundamental changes in people’s lives, such as making healthy food more available, creating safe places for kids to be more active, and spreading awareness through education and local policies. By focusing on entire communities rather than solely on individuals, public health initiatives enable families to make healthier, more sustainable choices. This approach can meaningfully reduce childhood obesity rates and prevent many of the health problems that often come with obesity.
The socioecological model provides a fundamental framework for understanding how factors beyond individual choices, including a wide range of social and environmental influences, shape childhood obesity. At the personal level, a child’s knowledge and attitudes about food and exercise significantly influence obesity risk. However, these are often shaped by influences at other levels of the socioecological model. At the institutional level, schools or daycare centers may lack access to nutritious meals, physical education, or other health-related resources. At the community level, additional barriers emerge–especially in low-income areas of Houston–where families may live in food deserts or neighborhoods without safe outdoor spaces (Boyd, 2019; Campbell, 2016). Lastly, policy-level factors, including federal nutrition programs and public health funding, directly affect the resources available to these communities (Campbell, 2016). By examining childhood obesity through this framework, we can better identify the structural causes of these more profound health disparities and design public health interventions that extend beyond clinical settings to promote more equitable change.
Methods
After reviewing 21 peer-reviewed journal articles and scholarly sources from government reports, Google Scholar, and PubMed, we conducted a literature review to identify gaps and limitations in current interventions that may prevent children from receiving effective obesity care. The literature review examines the significant risk factors for childhood obesity, existing interventions, the most affected Houston communities, and the growing prevalence of the condition throughout the United States. We did not explore in depth whether pollutants and other environmental conditions contribute to obesity, as there is limited research on how urban environments–such as Houston–can affect a child’s metabolism.
Dr. Deanna Hoelscher was selected as a key stakeholder based on her direct influence, expertise, and active involvement in addressing childhood obesity in Houston. Dr. Hoelscher serves as the Principal Investigator for the Texas School Physical Activity and Nutrition (Texas SPAN) survey, an initiative funded by the Texas Department of State Health Services to monitor the prevalence of obesity in school children across Texas, and the STREETS project, a National Institute of Health (NIH) funded cultural experiment examining how safe routes influence school policies related to physical activity.
Based on Dr. Hoelscher’s insights, we decided to develop a digital platform featuring hands-on tutorial videos, educational resources, and interactive workshops to help families learn by doing. This approach aligns with her emphasis on practical skill-building and active learning, allowing families to adopt and maintain healthier habits.
Literature Review
In the past two decades, childhood obesity rates have increased by 50% percent. In 2025, one out of ten children is considered obese, affecting a total of 188 million children worldwide (Obesity Exceeds Underweight for the First Time among School-Age Children and Adolescents Globally – UNICEF, 2025). There are multiple causes of this increase in obesity rates. According to the Future of Children Journal, fewer children walk to school today than they did in the 1970s, and increased access to high-calorie foods further contributes to childhood obesity (Anderson et al., 2006).
Children most at risk for obesity are commonly those who are from households that are low-income and/or receive government assistance. A study conducted by the Texas Childhood Obesity Research Demonstration (TX CORD) found that overweight fifth graders were more likely to receive SNAP benefits and had fewer recreational opportunities (Campbell et al., 2016).
Our research team consists of members from Illinois, Pennsylvania, Texas, and California, with the most disproportionate findings reported in Houston, Texas. In 2019, approximately 34% of high school students in Houston were classified as overweight or obese, exceeding both state and national averages (Boyd, 2019). The national average for childhood obesity is 19.7% (CDC, 2024). In Harris County, the obesity rate was about 34% among children aged 12 or older (Preventing Childhood Obesity: A Guide for Houston Families – Elite Hospital Kingwood, 2025). These trends reflect a significant public health concern, especially in underserved neighborhoods. Hispanic and Latino children face nearly double the obesity risk compared to non-Hispanic white children in Texas (UTHealth, Child Obesity Prevalence in Texas). Nationally, obesity prevalence increased as family income decreased, with rates rising from 11.5% among children in households earning more than 350% of the federal poverty level (FPL) to 25.8% among those at or below 130% of FPL (CDC, 2024).
Individual risk factors for childhood obesity include genetic predisposition, dietary patterns, physical activity levels, and socioeconomic status. The Viva la Family Study, conducted among Hispanic families in Houston, found substantial heritability for body composition and lifestyle behaviors, suggesting that genetics significantly contributes to obesity risk (Butte et al., 2006). Additionally, the TX CORD study revealed that children whose mothers are obese were more than four times as likely to have severe obesity. Children from low-income families frequently face multiple health challenges, which contribute to higher rates of obesity and chronic disease. First, food insecurity and restricted access to affordable, nutritious foods can contribute to poor dietary habits, such as excessive consumption of sugar-sweetened beverages and low intake of fruits and vegetables (Salahuddin et al., 2017). Second, physical inactivity is more common in low-income neighborhoods, where budgetary restrictions and a lack of safe recreational spaces limit options for exercise and extracurricular activities (Salahuddin, 2017). Finally, low parental educational levels may lead to lower health literacy, which can reduce awareness of nutrition and physical well-being, reinforcing unhealthy habits (Maia et al., 2025).
At the interpersonal level, family dynamics, parenting styles, and social support systems play a crucial role in the development and management of childhood obesity. Research by NIH on low-income families suggests that specific parenting approaches, such as restricting food intake to control picky eaters, may directly affect children’s weight status (NIH, Does parenting affect children’s eating and weight status?). Additionally, a study by UTHealth Houston involving parents of young children with early-onset obesity identified significant interpersonal barriers: conflicting advice from family members, stigma from medical professionals, and lack of support at home. These challenges often lead to parental isolation and increased stress when attempting to implement dietary changes (Bryant et al., 2022).
Misinformation within families, such as the idea that high-protein foods are good for you, can also undermine healthy behavior. When families do not model healthy eating or prioritize physical activity, children are less likely to develop those habits. In neighborhoods where safety is a concern, outdoor play is restricted, leaving children to engage in screen-based activities for recreation. Peer influence and a lack of supportive relationships can further discourage health behaviours, especially when unhealthy food and sedentary habits are normalized in school and social environments (Salvy et al., 2012).
Many organizations, such as BOUNCE and the Texas Department of Health and Human Services, have been instrumental in reducing childhood obesity rates through educational campaigns and community intervention. These organizations partner with schools and nonprofits to implement programs such as after-school activity opportunities and nutrition education. The BOUNCE program at the University of Houston works with the community to reduce obesity related diseases by promoting healthy eating, regular physical activity, and body positivity among low-income Hispanic and African American Children through its summer program (Bounce & About, 2024). Similarly, the CAN DO program, which focused on integrating physical activity and nutrition education into the school curriculum of children in the Sunnyside and Magnolia Park communities of Houston led to more than 400 children and family members attending fitness events and an average of 48 students per after-school program (Correa et al., 2010). Despite these initiatives, safety concerns and transportation barriers can still limit children’s access to parks and recreational activities.
Various community-based factors influence childhood obesity rates in Houston, including access to recreational space, socioeconomic status, and the availability of healthy food options. According to the 2021-2023 Texas SPAN (School Physical Activity and Nutrition) Survey, nearly half of second- and fourth-grade students did not play outside on at least five days a week (Childhood Obesity Prevalence in Texas after COVID: Findings from the 2021-2023 Texas SPAN Survey, n.d.). Additionally, almost all school-aged children in the state fail to meet physical activity guidelines established by the Texas Education Agency (TEA) (Childhood Obesity Prevalence in Texas after COVID: Findings from the 2021-2023 Texas SPAN Survey, n.d.). While these are significant challenges, several Houston-based organizations are working to help children and their families build healthy habits from an early age. For example, Legacy Community Health discusses the importance of physical activity and proper nutrition with parents during pediatric visits regardless of the child’s weight (Boyd, 2019). This proactive approach helps normalize conversations regarding healthy lifestyles, encouraging early prevention of childhood obesity. Texas Children’s Hospital, the nation’s largest children’s hospital, also contributes to prevention efforts by offering free general nutrition counseling and behavior-modification programs for children and their families (Obesity and Weight Management; Texas Children’s Hospital, n.d.). These programs aim to support low-income families and their children in developing sustainable lifestyle changes alongside medical professionals and nutritionists.
In Houston, local and state policies directly impact care, access, funding, and support for childhood obesity prevention, especially among low-income immigrant families. For example, programs such as CATCH (Coordinated Approach to Child Health) and CAN DO Houston, which are backed by local government initiatives, are both community efforts that significantly impact the prevalence and management of childhood obesity. CATCH, implemented in thousands of schools and supported by district wellness policies, promotes healthier meals and daily physical activity to reduce obesity risk. CAN DO Houston, led by the city’s health department, emphasizes neighborhood-level improvements such as school healthy food gardens and access to fresh food. These policies help manage and reduce obesity prevalence by making healthy choices more accessible. However, gaps remain in implementation and reach. Many families are unaware of available resources due to language barriers and concerns related to immigration status. Not all neighborhoods benefit equally, either. Expanding these programs even more citywide, improving outreach, and ensuring equitable access across communities would strengthen their effectiveness. Addressing obesity early is particularly important because long-term obesity has been linked to increased risk of neurodegenerative diseases, such as Alzheimer’s, due to chronic inflammation (Kueck et al., 2023).
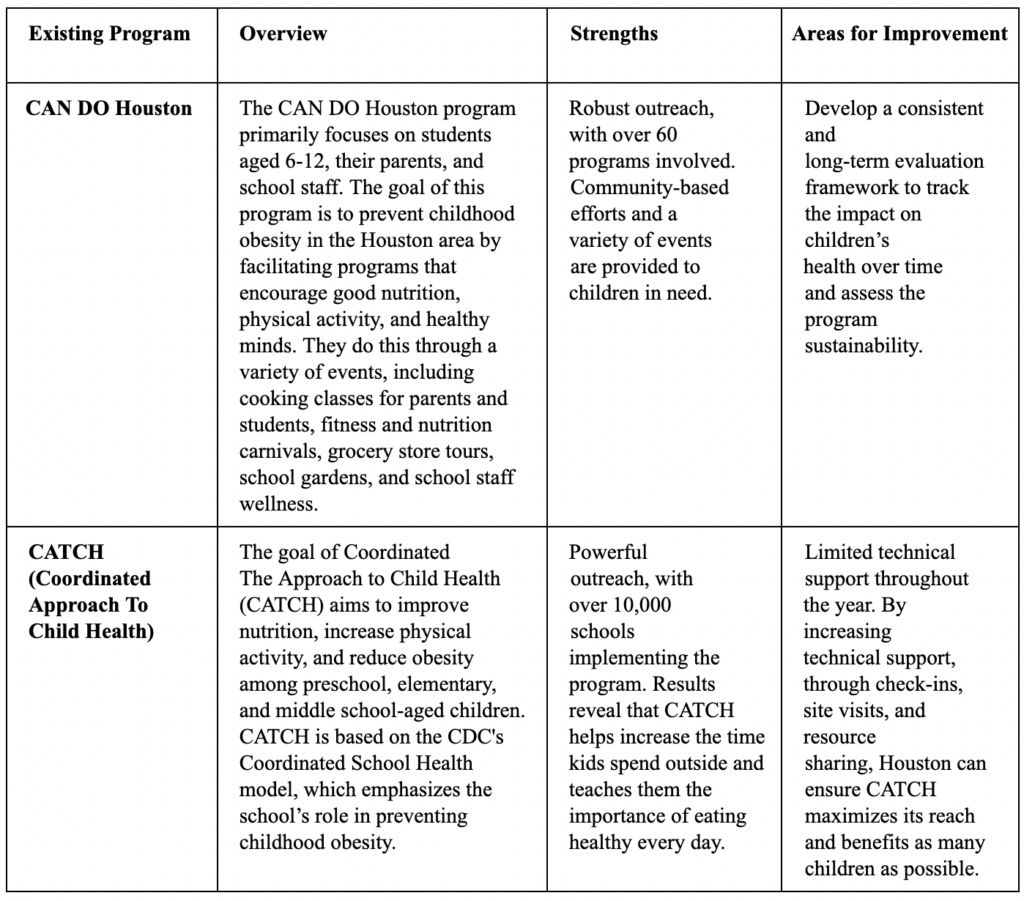
Table 1: Overview of Childhood Obesity Programs for Low-income and Immigrant Families in Houston
Stakeholder Perspectives
Through an interview with Dr. Deanna Hoelscher, a researcher at UT Health Houston’s School of Public Health, we identified several social perspectives on treating childhood obesity in Houston. First, Dr. Hoelscher acknowledged the importance of school-based cooking and physical activity programs that promote active learning, which allows families to “learn by doing”. One of the most important takeaways was that families should focus on how to apply new nutrition knowledge rather than what foods are healthy. This form of cooking education, facilitated by Catch Global Foundation, helps to establish practical skills and facilitate long-term behavior change. Dr. Hoelscher further identified the impact of misinformation about obesity, including common myths that high-protein diets and saturated fats are always healthy. She emphasizes a demand for more open education to build trust and habits. In terms of technology, Dr. Hoelscher suggests that digital tools are more effective when they are interactive, such as personalized reminders or interactive video content (e.g., box breathing, snack-making, exercise streams). UTHealth Houston’s Nourish programs were cited as successful examples of synthesizing technology with real-life applications.
Digital Health Solutions
The Quintuple Aim, a digital solution, offers a clear framework for addressing childhood obesity in Houston, specifically in low-income communities. By focusing on improving population health, the model pushes efforts toward prevention and early support for children and families. Enhancing the patient experience ensures that care is accessible and responsive to individual needs. The model also emphasizes improving the healthcare provider experience by recognizing that better tools and workflows allow providers to deliver care more effectively. Most importantly, it centers on advancing health equity by addressing social and environmental factors that impact health outcomes in underserved communities.
Additionally, the growing shift toward digital health solutions, like virtual care platforms, data-tracking tools, and mobile health services, is transforming how public and community health services are delivered. These technology-based solutions to public health problems make it easier to reach families where they are. These innovations support the goals of the Quintuple Aim by making care more efficient, particularly for populations facing systemic barriers.
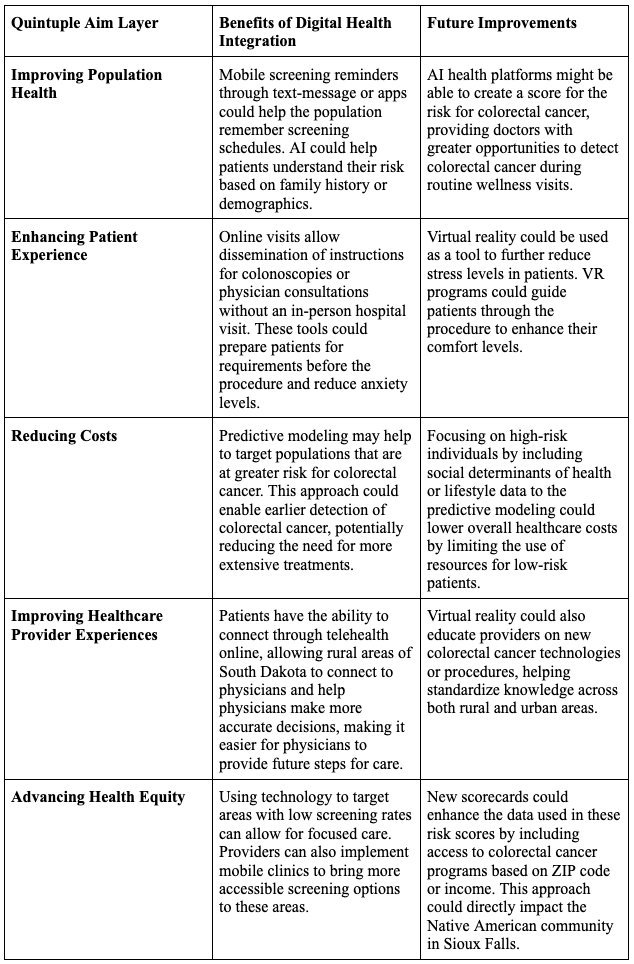
Table 2: Overview of Quintuple Aim Model
Plan of Action
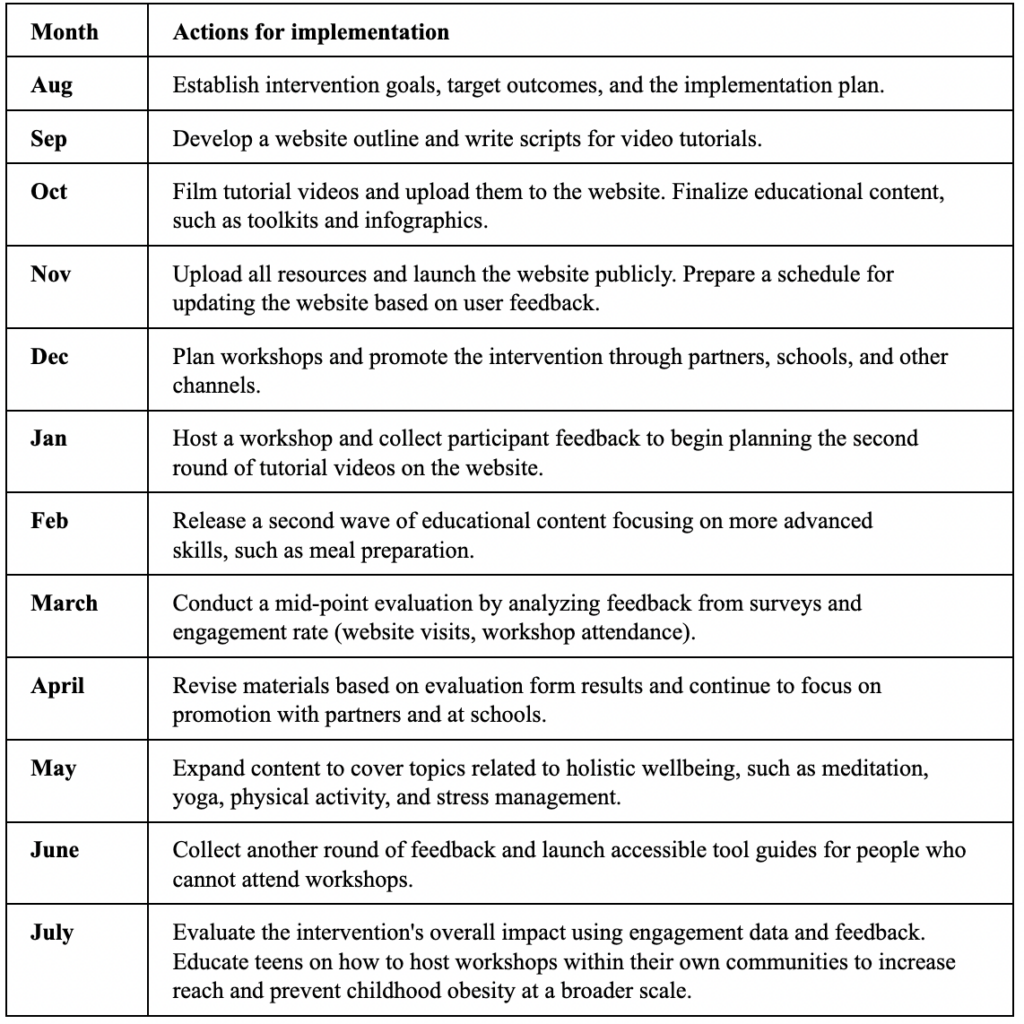
Table 3: Plan of Action
Plan of Action
The primary objectives of our intervention are to increase families’ nutritional literacy by 35% and to ensure that at least 50% of participants in the workshop series show improved physical activity levels. This intervention builds on what already exists in Houston while filling in key gaps that current programs have not fully addressed. Programs like CATCH and CAN DO Houston have made a meaningful impact in promoting healthier behaviors among children, especially in schools and neighborhoods. However, gaps in outreach still leave many low-income families (especially immigrant and minority communities) unaware or unable to benefit. Our literature review further suggests that early intervention is critical, not only for preventing obesity but also for reducing long-term risks like chronic inflammation and neurodegenerative diseases that can result as a major side-effect of obesity.
Our plan builds on existing work by adding hands-on, family-focused resources, such as workshops and tutorial videos, that support behavior change in the home and community, not just in schools. This way, families can practice and personalize what they learn, which helps our intervention be applied in real life. This approach strengthens what is already working in Houston while addressing the remaining barriers. Moreover, this intervention also aligns with the Quintuple Aim framework by promoting overall population health and advancing health equity by addressing the specific needs of underserved communities.
According to Dr. Hoelscher, when individuals have regular opportunities to practice and customize healthy habits in contexts that are important to them, those habits are more likely to stick. The addition of active experiences, such as cooking meals together in the evening, gentle physical activities like stretching or walking, and mindfulness practices like box breathing, helps these families adopt healthier lifestyles. Dr. Hoelscher also recommended interactive formats that guarantee skill-building. For example, rather than merely telling a person to eat better, stakeholders insisted on showing them how, with easy-to-follow recipes, group preparation of dishes, and explorations into inexpensive healthy foods. Physical and mental well-being were often mentioned together in these debates, with yoga, breathing exercises, and movement therapy suggested as easy-to-apply tools that will improve both. Dr. Hoelscher also supported incentive-based approaches, such as rewards for overcoming obstacles or for participating in health contests such as walking clubs. Such strategies, she noted, enhance health education by making it more sustainable and engaging, particularly in communities where individual motivation may be lower.
Strengths and Limitations
Discussion
In Houston, Texas, childhood obesity is more common among the Hispanic and Latino population. This is due to multiple factors, including low income and limited access to grocery stores and nutrition information. It is crucial to approach this problem with multiple solutions, including preventive measures and efforts to improve health in at-risk areas. Healthcare providers can provide early screening for obesity, which serves as a preventive measure. Education is also essential, as obesity prevention is closely tied to the community’s ability to care for its health.
Nutrition curricula in schools, especially in underserved towns, can help children understand their food choices and their effects. Digital tools can be used to track and record data, which further helps identify communities at risk of high childhood obesity rates. Our intervention increases access and equity by not simply listing information but instead providing hands-on tutorial videos and interactive workshops, helping families learn the basics of putting together a healthy meal plan from the comfort of their devices. Additionally, hosting classes in person will foster a community environment and encourage children to maintain the habits they have acquired. The online workshop system will also provide greater flexibility for parents who may not be able to attend an in-person event.
Conclusion
Childhood obesity is a significant public health issue affecting millions of families in the United States (Sanyaolu et al., 2019). In Houston, TX, obesity rates among children are particularly high due to poor eating habits and a lack of physical activity, specifically in lower-income communities (UTHealth, Child Obesity Prevalence in Texas). Our proposed intervention will improve public health practices by increasing nutritional literacy and promoting healthy habits. The intervention involves developing a website featuring hands-on tutorial videos and interactive workshops to encourage families to adopt healthier habits in their daily lives. By using a holistic approach and digital health tools, the project will also help reduce language barriers and promote accessibility. If successful on the local level, this intervention can be expanded to communities across the nation, helping to prevent childhood obesity on a broader scale.
References
- Anderson, P. M. & Butcher, K. F. Childhood obesity: trends and potential causes. Future Child. 16, 19–45 (2006).
- Bounce. About Bounce. University of Houston https://uh.edu/education/bounce/about/ (2024).
- Boyd, C. Tackling childhood obesity in the Houston area. Legacy Community Health https://www.legacycommunityhealth.org/newsblog-tackling-childhood-obesity-in-the-houston-area/ (2019).
- Brighter Bites. SNAP-Ed intervention profile. SNAP Education Connection https://snaped.fns.usda.gov/library/intervention/brighter-bites (n.d.).
- Bryant, K. et al. Isolation in a sea of “experts”: identifying the parental struggles caring for children with early-onset obesity. Childhood Obesity 19, 408–416 (2023).
- Butte, N. F., Cai, G., Cole, S. A. & Comuzzie, A. G. Genetic and environmental contributions to childhood obesity in Hispanic populations: the Viva la Familia Study. Am. J. Clin. Nutr. 84, 646–654 (2006).
- Campbell, M. K. Biological, environmental, and social influences on childhood obesity. Pediatr. Res. 79, 205–211 (2016).
- Childhood obesity prevalence in Texas after COVID: findings from the 2021–2023 Texas SPAN survey. University of Texas Health Science Center https://sph.uth.edu/research/centers/dell/legislative-initiatives/docs/Childhood%20Obesity%20%20LL.pdf (n.d.).
- Centers for Disease Control and Prevention. Childhood obesity facts. https://www.cdc.gov/obesity/childhood-obesity-facts/childhood-obesity-facts.html (2024).
- Correa, N. P. et al. CAN DO Houston: a community-based approach to preventing childhood obesity. Prev. Chronic Dis. 7, A88 (2010).
- GBD 2021 US Obesity Forecasting Collaborators. Prevalence of overweight and obesity in the USA, 1990–2021, with forecasts to 2050. Lancet 404, 2278–2298 (2024).
- Kueck, P. J., Morris, J. K. & Stanford, J. A. Obesity and neurodegeneration: links and risks. Degener. Neurol. Neuromuscul. Dis. 13, 111–129 (2023).
- Maia, C. et al. Impact of parental behaviors on children’s lifestyle, mental health, and BMI: a scoping review. Children 12, 203 (2025).
- Obesity and weight management. Texas Children’s Hospital https://www.texaschildrens.org/departments/obesity-and-weight-management (n.d.).
- UNICEF. Obesity exceeds underweight for the first time among school-age children and adolescents globally. https://www.unicef.org/press-releases/obesity-exceeds-underweight-first-time-among-school-age-children-and-adolescents (2025).
- Houston State of Health Data Portal. Coordinated approach to child health (CATCH). https://www.houstonstateofhealth.com/promisepractice/index/view?pid=3612 (n.d.).
- Preventing childhood obesity: a guide for Houston families. Elite Hospital Kingwood https://elitekingwood.com/childhood-obesity-problem/ (2025).
- Salahuddin, M. et al. Predictors of severe obesity in low-income Hispanic/Latino children. Prev. Chronic Dis. 14, E141 (2017).
- Salvy, S.-J., de la Haye, K., Bowker, J. C. & Hermans, R. C. J. Influence of peers on eating and activity behaviors. Physiol. Behav. 106, 369–378 (2012).
- Sanyaolu, A. et al. Childhood and adolescent obesity in the United States: a public health concern. Glob. Pediatr. Health 6, 1–11 (2019).
Related Posts
Incarceration and Motherhood: A Brief Overview of Maternal Health Issues in American Prisons
Figure 1: Guards in prisons are able to put prisoners...
Read MoreMind Missing Out? Fear of Missing Out and the Brain
Figure: A person scrolling through news articles on their smartphone....
Read MoreHow Many Humans Does it Take to Host a Planet?
Figure 1: This is an artist’s rendering of a potential...
Read MoreGender Differences in Health and Medicine and the Importance of Gender-Specific Medicine in Healthcare Policy
This article was originally submitted to the Modern MD competition...
Read MoreTo safeguard Africa’s topmost predators
From Nepal’s bengal tiger to Kenya’s big Lions, conservation of...
Read MoreDarius Dastur, Mishal Ali, Harshitha Ezhilarasan, Hasan Khan, Aaron Akasala