This publication is produced in partnership with Project UNITY’s Catalyst Academy Class of 2025, a student public health research and education program.

Abstract
Adolescents aged 13–17 in Baltimore County, Maryland have experienced significant declines in physical activity and sleep quality, particularly since the onset of the COVID-19 pandemic. These two health behaviors are closely linked and essential for healthy development, yet both have deteriorated due to disrupted routines, increased screen time, and reduced access to structured physical activity. This study seeks to investigate how the pandemic affected the relationship between physical activity and sleep among adolescents and to explore how social determinants of health (SDOH) and community-level disparities influence this issue in Baltimore County. Using databases such as PubMed, Google Scholar, and government websites, our group identified 60 sources and closely reviewed 22 peer-reviewed articles published within the last decade. Selection criteria prioritized studies that examined the intersection of adolescent sleep, physical activity, mental health, and the COVID-19 pandemic. Additionally, stakeholder interviews were conducted with public health nurses, sleep medicine specialists, and community leaders to contextualize the findings. Results indicate that low-income and racially marginalized adolescents in Baltimore County are higher/greater at risk due to environmental stressors, inadequate school resources, and unsafe or inaccessible spaces for recreation. Existing interventions often fail to address the connection between sleep and physical activity and are frequently unaffordable or distributed inequitably. To resolve this, our proposed intervention implements a hybrid in-person and digital model to promote adolescent sleep hygiene and physical activity through themed wellness challenges, fitness classes, and social media engagement. This approach emphasizes accessibility, engagement, and sustainability to support adolescent well-being locally and potentially in similar urban communities nationwide.
Keywords: Intervention; physical activity; sleep quality; adolescent; disparities; COVID-19 pandemic
Introduction
The COVID-19 pandemic, which spanned from March 2020 to May 2023, significantly disrupted the daily routines of adolescents, particularly affecting their levels of physical activity and quality of sleep. For youth aged 13 to 17, these disruptions have led to both immediate and long-term health concerns, including increased risks of obesity, chronic disease, stress, and mental health challenges. As public health practitioners, it is crucial to understand how this unprecedented period altered adolescent health behaviors and outcomes. This paper explores the question: How did the COVID-19 pandemic affect the relationship between physical activity and sleep quality among adolescents living in Baltimore County, Maryland? To guide this analysis, key terms such as “intervention” (a public health program or strategy aimed at improving outcomes), “physical activity” (any bodily movement that promotes health), “sleep quality” (the effectiveness and restfulness of sleep), and “disparities” (inequities in health outcomes among different groups) were defined.
By investigating the impact of the pandemic on this specific population, this paper aims to contribute to the development of more effective and equity-focused public health interventions. Using a public health lens, this paper first provides background on the importance of sleep quality and physical activity for adolescent health. It then outlines the methodology and reviews current literature on this topic. Drawing on stakeholder perspectives and exploring digital health solutions, a proposed intervention is presented to address the dual challenges of reduced physical activity and poor sleep quality. The potential strengths, limitations, and community impact of this proposed approach is then discussed. Ultimately, this paper offers insights and preliminary conclusions that may inform future efforts to support adolescent well-being in the post-pandemic period and beyond.
The Importance of a Public Health Lens
Examining the correlation between sleep quality and physical activity in 13-17 year olds in Baltimore County using a public health framework is crucial, as this issue affects a dense population of adolescents and contributes to detrimental health consequences. The COVID-19 pandemic caused major disruptions in adolescents’’ daily routines, with physical activity significantly reduced due to school closures, lockdowns, and remote learning. As a result, sleep quality declined, negatively affecting overall physical and mental health of teenagers. Taking a public health approach to this topic allows for the identification of its specific root causes and the development of proactive and preventative measures, such as promoting youth fitness programs and advocating for healthy sleep habits. Additionally, tackling this issue at a county level allows interventions to directly target the population’s needs while raising awareness. Ultimately, this framework also ensures that interventions are equitable, so adolescents in underserved areas of Baltimore County are fairly represented.
The socio-ecological model (SEM), a framework that breaks down influential factors on human health into various levels, allows us to uncover health inequities that extend beyond clinical diagnosis. When patients refer to medical professionals seeking a resolution, medical professionals must ask themselves: why, and how is this problem occurring? The SEM takes into account multiple layers, including individual behavior, societal effects, and policy-related impacts. For instance, when adolescents experience inadequate sleep, it is often not solely due to poor time management, but rather a combination of factors such as stressful environments, early school start times, and limited access to safe spaces for physical activity and stress management. By examining these interconnected levels, the SEM illustrates income, neighborhood safety, family expectations, school pressures, and stigma surrounding mental health contribute to poor sleep quality. This perspective further demonstrates that effective public health solutions must look past clinical diagnosis and address systems in which individuals live.
Methods
60 articles were extracted, primarily consisting of peer-reviewed studies from scholarly journals accessed through PubMed or Google Scholar, all of which pertained to physical activity or sleep. Additionally, government and state department websites, including the US Department of Health and Human Services and HealthyPeople.gov, were used to obtain public health reports. The latest policy reports regarding the topic were also retrieved from the American Public Health Association. Of the 60 articles identified, 22 articles were selected for in-depth review based on their focus on the intersections of mental health, physical activity, and sleep, as well as their relevance to the COVID-19 pandemic and the topic.
Stakeholders were chosen after analysis of which perspectives would be most relevant to understanding sleep hygiene and its effects on physical health. The team first identified pediatricians, physical therapists, sleep specialists, and other similar professionals to be most aligned with the research goals, as these groups work closely with children and adolescents. Stakeholder interviews with two specialists provided important insights on sleep health and sleep-related policies in Maryland, informing the proposed plan of action, which was designed to address the issue at the community, organizational, and policy levels, while also prioritizing implementation feasibility and ethics.
Literature Review
National Trends and Epidemiology: Sleep hygiene and physical activity are essential to adolescent development, yet both have declined across the United States. Currently, 82% of adolescents report poor sleep quality, and only 20% meet national guidelines for aerobic and muscle-strengthening activities (Şimşek & Tekgül, 2019; “Physical Activity,” n.d.). These trends are linked to rising rates of depression, anxiety, and other health challenges (Firth et al., 2020; Sejbuk et al., 2022). Adolescents from urban and disadvantaged backgrounds, particularly those from lower socioeconomic or racially marginalized groups, are disproportionately affected (Rockette-Wagner et al., 2017; Nahmod et al., 2022). The COVID-19 pandemic further exacerbated these issues, as lockdowns disrupted school-based physical activity and increased screen time, resulting in worsened sleep quality and reduced movement. These effects have persisted to date, with no clear signs of recovery (Cortez et al., 2023; Do et al., 2022; Luciano et al., 2021).
Social Determinants of Health: Multiple social and environmental factors contribute to these trends. Economic instability can lead to chronic stress and irregular work schedules, thereby limiting opportunity for exercise and sleep. Lower-income families often lack access to safe recreational spaces and nutritious food, both of which are key to physical and mental health (Lundahl et al., 2013; Gillis et al., 2023). Educational disparities also play a role, as underfunded schools may lack physical education programs or health literacy resources, which are often the first to be cut during budget shortfalls (Craig, 2024; Supporting Physical Education in Schools for All Youth, 2021). Healthcare access is another barrier: adolescents without regular medical care may go undiagnosed for sleep or physical health issues. Urban environments, where many adolescents reside, often present additional challenges, including overcrowding, limited green space, and higher crime rates (Hasson et al., 2021). During the pandemic, fitness center closures led to a 32–48% drop in physical activity (Dunton et al., 2020). Furthermore, social media has contributed to unhealthy sleep habits and toxic fitness messaging, further disrupting adolescent health behaviors (Fobian et al., 2016; Royant-Parola et al., 2018).
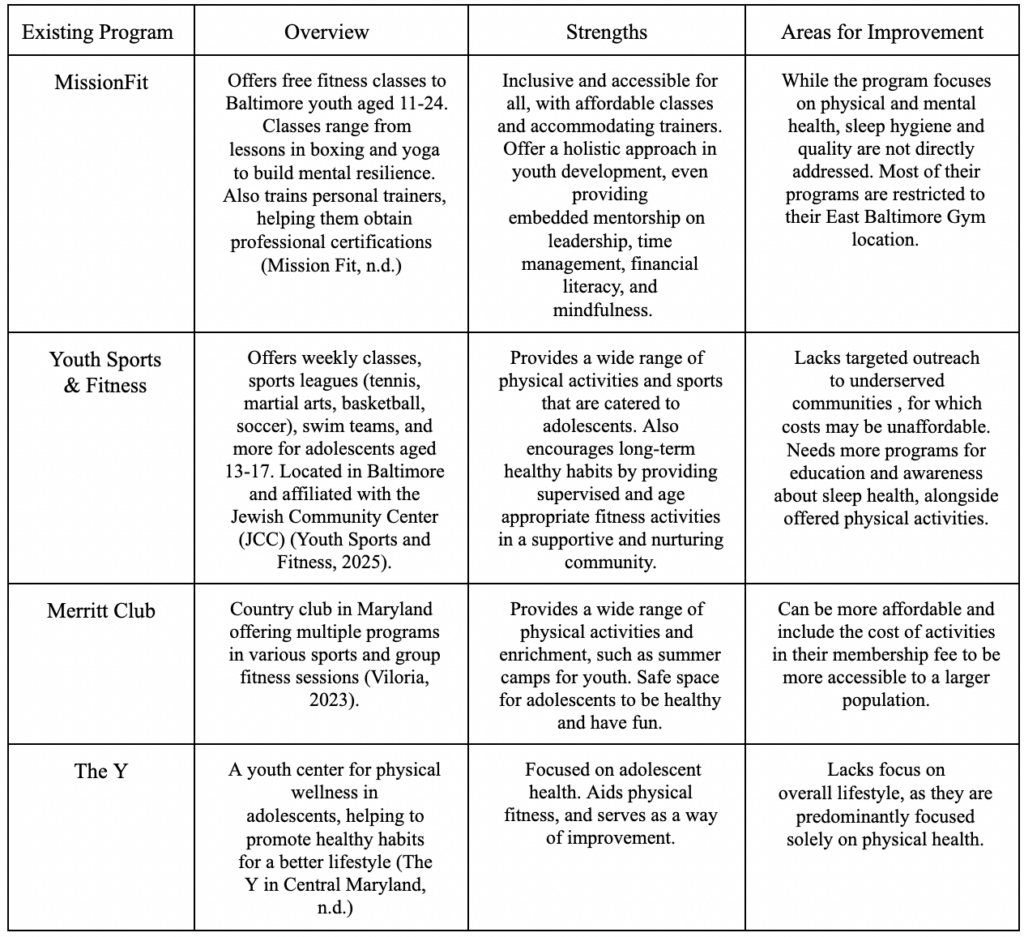
Table 1: Overview of Sleep and Physical Activity Programs for Adolescents Aged 13-17 in Baltimore County
Stakeholder Perspectives
In developing our intervention, several key stakeholders, whose insights helped shape understanding of adolescent health during and after the COVID-19 pandemic, were consulted. Shri Ji, founder of the nonprofit Shri Yoga, emphasized how the pandemic disrupted physical activity and mental well-being, particularly among adolescents. His organization, which offers over 70 weekly yoga classes, observed that practices such as yoga helped teens manage stress and improve sleep during lockdowns. He noted that even virtual yoga sessions provided adolescents with a sense of connection and calm, reinforcing the idea that a rested mind supports a rested body.
Additional public health experts echoed these concerns and provided complementary perspectives. Rose Burrell, BSN, RN, Public Health Nurse Administrator and Chief of Population Health for Baltimore County, highlighted/emphasized the foundational importance of sleep in adolescent development, noting its effect on mental health, physical health, and academic performance. She recommended leveraging social media influencers to effectively engage teenagers in health promotion efforts. Dr. Katherine Maul Buki, a sleep medicine specialist, reinforced the importance of sleep quality by citing research linking adequate sleep to injury prevention, improved cognitive function, and increased traffic safety. She further discussed innovative technologies, including CBT-I apps, telehealth, and AI-powered tools, that are transforming sleep care. Lastly, Sherrie Phillips Byers, MSN, RN, explained how pandemic-related disruptions to adolescent routines continue to affect youth today, making structured interventions increasingly important.
Digital Health Solutions
The Quintuple Aim model provides a framework for public health advocacy through the lens of five major goals that include population health enhancement, patient experience improvement, cost reduction, healthcare provider support, and health equity advancement. In Baltimore County, SDOH such as income, housing insecurity, and transport impact health differently. The model specifically allows for the redirection of technological advancement to more effectively reach marginalized populations experiencing poor sleep quality. Today, advanced technology (including telecommunication, mobile health apps, remote monitoring systems, and AI-assisted decision tools), offer promising opportunities to address gaps in adolescent care, particularly for those in disadvantaged neighborhood families. These technologies can be leveraged to enhance sleep quality for adolescents through virtual fitness classes and physical activity promotion campaigns. Such tools are relatively low cost, widely accessible, and help reduce strain on healthcare systems by emphasizing prevention. By effectively applying the Quintuple Aim model, the proposed intervention can make healthcare more accessible and efficient for the target population.

Table 2: Quintuple Aim of Healthcare
Plan of Action
The proposed intervention targets adolescents in underserved communities, particularly in Baltimore County, Maryland, who are disproportionately affected by sleep disparities. The initiative aims to improve both sleep hygiene and physical activity through education, engagement, and community-based programming. By encouraging adolescents to participate in physical activities and educating them on the importance of sleep, we seek to foster sustainable healthy habits
The intervention began in August 2025 with the development of workshop materials and outreach to community partners, including local high schools and fitness programs. A community needs assessment survey was launched to gather data on current sleep and activity habits. In September, a social media presence was established on Instagram, TikTok, Facebook, and LinkedIn to promote the initiative. Inspired by the 2025 revival of the UNC Ice Bucket Challenge, wellness challenges were designed to encourage engagement through a ripple effect. Recruitment of certified instructors and volunteers also began during this phase.
By October, the first in-person and virtual fitness classes were launched, beginning with a free yoga session. Subsequent classes were priced at five dollars to cover administrative costs and supplies, while merchandise sales served as both a fundraising and awareness tool. Weekly classes hosted in partnership with a local yoga studio focused on various aspects of physical health, such as cardiovascular fitness, core strength, and bone density. Social media campaigns continued to run in parallel and were designed to align with seasonal events to keep participants engaged.
In December, the “Winter Glow-Up” campaign was introduced to encourage participation in preparation for the new year. January’s theme, “New Year, New Me,” leveraged seasonal goal-setting, incorporating movie-themed classes chosen by participants. February’s “Healthy Heart, Healthy Me” campaign focused on cardiovascular health, March’s “Move Your March” encouraged student activity
During a demanding academic period, April featured dual themes—“Get Ready for Prom” for upperclassmen and “Spring into Action” for underclassmen—with playful class activities tied to April Fools’ Day. Progress was monitored through attendance records, class engagement, merchandise sales, and post-session surveys.
In May, during exam season, the focus shifted to promoting sleep hygiene via digital platforms. A social media campaign encouraged adolescents to obtain at least eight hours of sleep per night, highlighting the cognitive benefits of rest and the risks of sleep deprivation. In-person classes were paused, while expert advice and stress-management strategies were shared online. Collaborations with local influencers and organizations were further explored to amplify outreach.
As summer approached, the focus returned to physical activity and social engagement. During June and July, outdoor exercise and group activities were promoted through social media challenges, and virtual fitness sessions increased to twice weekly. Partnerships with local fitness centers facilitated workshops and explored free teen membership possibilities. These efforts aimed to increase accessibility and enjoyment of physical activity during the summer, but also required additional coordination with community partners for venues and staffing.
August marked the evaluation phase of the intervention. Social media metrics, class attendance, and survey responses were analyzed to assess overall effectiveness. A final community survey gathered anonymous feedback to inform future improvements. This data and insights from throughout the year will be for use for future community leaders and intervention teams. By sharing findings, this initiative aims to support the development of sustainable, scalable programs adaptable to other communities facing similar challenges.
Discussion
The strengths of the intervention lie in its interactive and engaging design. A unique feature of this program is the incorporation of seasonal themes, combating one of the main challenges of physical activity: consistency. Social media further supports this by providing updates on challenges and fostering a strong community around physical wellness. Additionally, this intervention provides value for the by targeting adolescents, helping cultivate a future healthier community in the Maryland area. Accessibility is also a key strength, with a combination of synchronous and asynchronous programming.
However, there are some limitations. Maintaining motivation remains a potential challenge for an asynchronous audience, who may be less inclined to stay active compared to its synchronous counterpart. Nevertheless, building an engaging, community-driven physical wellness program can help to sustain consistent engagement throughout the year.
Conclusion
Sleep quality and physical activity were significantly affected by the COVID-19 pandemic, leading to lasting impacts on mental health and physical well-being. Baltimore County, with its diverse urban population, is particularly at risk unless meaningful interventions are implemented. The proposed action plan aims to lay a foundation for future programs that increase physical activity and improve sleep quality. By using a social media campaign that speaks the language of our target audience and promotes physical activity challenges, this intervention hopes to encourage sustainable and enjoyable habits. While the effects may not reach everyone, future efforts should target policy-level change for more permanent changes . Addressing sleep quality and physical health is essential, and future research should continue exploring innovative solutions to fill gaps in current interventions.
References
- Becker, S. P. & Gregory, A. M. Editorial perspective: Perils and promise for child and adolescent sleep and associated psychopathology during the COVID-19 pandemic. J. Child Psychol. Psychiatry 61, 757–759 (2020). https://doi.org/10.1111/jcpp.13278
- Cortez, C. A. et al. Moderate-to-vigorous intensity physical activity among U.S. adolescents before and during the COVID-19 pandemic: Findings from the Adolescent Brain Cognitive Development Study. Prev. Med. Rep. 35, 102344 (2023). https://doi.org/10.1016/j.pmedr.2023.102344
- Craig, D. W. et al. Whole-of-school physical activity promotion: Findings from elementary schools in the United States. Am. J. Prev. Med. (2024). https://doi.org/10.1016/j.amepre.2024.08.003
- Do, B., Kirkland, C., Besenyi, G. M., Smock, M. C. & Lanza, K. Youth physical activity and the COVID-19 pandemic: A systematic review. Prev. Med. Rep. 29, 101959 (2022). https://doi.org/10.1016/j.pmedr.2022.101959
- Dunton, G. F., Wang, S. D., Do, B. & Courtney, J. Early effects of the COVID-19 pandemic on physical activity locations and behaviors in adults living in the United States. Prev. Med. Rep. 20, 101241 (2020). https://doi.org/10.1016/j.pmedr.2020.101241
- Firth, J. et al. A meta-review of lifestyle psychiatry: The role of exercise, smoking, diet and sleep in the prevention and treatment of mental disorders. World Psychiatry 19, 360–380 (2020). https://doi.org/10.1002/wps.20773
- Fobian, A. D., Avis, K. & Schwebel, D. C. Impact of media use on adolescent sleep efficiency. J. Dev. Behav. Pediatr. 37, 9–14 (2016). https://doi.org/10.1097/DBP.0000000000000239
- Gao, Y., Chen, S. & Bridle, C. Physical activity and mental health in children and adolescents during the COVID-19 pandemic: A meta-analysis. J. Sport Health Sci. 11, 285–295 (2022). https://doi.org/10.1016/j.jshs.2022.03.001
- Gillis, B. T., Hinnant, J. B., Erath, S. A. & El-Sheikh, M. Relationship between family income and trajectories of adjustment in adolescence: Sleep and physical activity as moderators. J. Adolesc. 95, 494–508 (2023). https://doi.org/10.1002/jad.12131
- Hasson, R. et al. COVID-19: Implications for physical activity, health disparities, and health equity. Am. J. Lifestyle Med. 16, 420–433 (2021). https://doi.org/10.1177/15598276211029222
- Mission Fit. Mission Fit https://missionfit.org/ (accessed 18 June 2025).
- Luciano, F., Cenacchi, V., Vegro, V. & Pavei, G. COVID-19 lockdown: Physical activity, sedentary behaviour and sleep in Italian medicine students. Eur. J. Sport Sci. 21, 1459–1468 (2021). https://doi.org/10.1080/17461391.2020.1842910
- Lundahl, A., Nelson, T. D., Van Dyk, T. R. & West, T. Psychosocial stressors and health behaviors: Examining sleep, sedentary behaviors, and physical activity in a low-income pediatric sample. Clin. Pediatr. 52, 721–729 (2013). https://doi.org/10.1177/0009922813482179
- Nahmod, N. G. et al. Neighborhood disadvantage is associated with lower quality sleep and more variability in sleep duration among urban adolescents. J. Urban Health 99, 102–115 (2022). https://doi.org/10.1007/s11524-021-00570-x
- Patrick, S. W. et al. Well-being of parents and children during the COVID-19 pandemic: A national survey. Pediatrics 146, e2020016824 (2020). https://doi.org/10.1542/peds.2020-016824
- U.S. Department of Health and Human Services. Physical activity. Healthy People 2030 https://odphp.health.gov/healthypeople/objectives-and-data/browse-objectives/physical-activity (accessed 18 June 2025).
- Rodriguez, J. How does the Affordable Care Act treat sleep apnea? Advanced Sleep Medicine Services https://www.sleepdr.com/the-sleep-blog/how-does-the-affordable-care-act-treat-sleep-apnea/ (2016).
- Rockette-Wagner, B. et al. Activity levels for four years in a cohort of urban-dwelling adolescent females. Med. Sci. Sports Exerc. 49, 695–701 (2017). https://doi.org/10.1249/MSS.0000000000001152
- Royant-Parola, S., Londe, V., Tréhout, S. & Hartley, S. The use of social media modifies teenagers’ sleep-related behavior. L’Encéphale 44, 321–328 (2018). https://doi.org/10.1016/j.encep.2017.03.009
- Rundle, A. G., Park, Y., Herbstman, J. B., Kinsey, E. W. & Wang, Y. C. COVID-19–related school closings and risk of weight gain among children. Obesity 28, 1008–1009 (2020). https://doi.org/10.1002/oby.22813
- Sejbuk, M., Mirończuk-Chodakowska, I. & Witkowska, A. M. Sleep quality: A narrative review on nutrition, stimulants, and physical activity as important factors. Nutrients 14, 1912 (2022). https://doi.org/10.3390/nu14091912
- Şimşek, Y. & Tekgül, N. Sleep quality in adolescents in relation to age and sleep-related habitual and environmental factors. J. Pediatr. Res. 6, 307–313 (2019). https://doi.org/10.4274/jpr.galenos.2019.86619
- American Public Health Association. Supporting physical education in schools for all youth. https://www.apha.org/policy-and-advocacy/public-health-policy-briefs/policy-database/2022/01/07/supporting-physical-education-in-schools-for-all-youth (2021).
- YMCA of Central Maryland. The Y in Central Maryland https://ymaryland.org/ (accessed 18 June 2025.
- Viloria, K. Downtown Baltimore gym & fitness center. Merritt Clubs https://merrittclubs.com/location/downtown-club/ (2023).
- Jewish Community Center of Greater Baltimore. Youth sports and fitness. https://www.jcc.org/program/youth-sports-and-fitness/ (accessed 2025).
Related Posts
Transgender Health Disparities in Prisons
Transgender people are targets for victimization within the prison system...
Read MoreInvestigating the Quality of Healthcare in Rural Areas
Cover Image: A rural Metro ambulance in Memphis, Tennessee. Rural...
Read MoreChildhood Unpopularity May Increase Risk of Cardiovascular Disease in Adulthood
Figure 1: Childhood experiences are widely considered to affect adult...
Read MoreAre We Driving Our Dogs Sick Through Our Urban Lifestyles?
Figure 1: Allergic disorders in humans and dogs are associated...
Read MoreThe Environmental Consequences of Civil Wars
Figure 1: This is the flag of Angola, the model...
Read MoreAre We Addicted to Social Media?
Cover Image: In the current age, social media has become...
Read MoreDarius Dastur, Mishal Ali, Harshitha Ezhilarasan, Hasan Khan, Aaron Akasala






