This publication is produced in partnership with Project UNITY’s Catalyst Academy Class of 2025, a student public health research and education program.

Abstract
Colorectal cancer is characterized by abnormal cell growth that originates in the colon or rectum. Polyps, or growths, occur on the inner lining of the large intestine and are most common in older individuals. A public health lens can be used to further investigate the recent increases in prevalence of this cancer in individuals aged 20-45 years old [1]. Current lack of public awareness results in lower survival rates and more cases being discovered at late stages beyond repair. A 2023 report by the American Cancer Society states, “colorectal cancer cases among adults younger than 55 increased from 11% (1 in 10) in 1995 to 20% (1 in 5) in 2019” [21]. We aim to raise awareness of colorectal cancer to help individuals recognize the risks and signs, and to provide them with the resources to prevent further progression of this disease. To do this, we extracted data from several sources that reflected South Dakota’s Sioux Falls, the location of the target population, and identified risk factors for this population. We gathered information from various stakeholders who discussed how this disease affects the community. The Sioux Falls area is at high risk for colorectal cancer due to poor diet patterns and rising rates of obesity. We focused on social context as a social determinant of health, as it contributes to delayed detection of colorectal cancer in younger adults.
Keywords: Colonoscopy; genetic mutations; immunochemical tests; oncologist; polyps; screening
Introduction
Colorectal cancer traditionally is a disease that predominantly strikes older adults, but a greater number of younger individuals aged 20-45 years old are being diagnosed each year [1]. It is now one of the most common and lethal cancers in the United States, as a developing health concern for young adults. Socially, individuals who lack consistent healthcare access, such as low-income families, rural residents, and American Indians are less likely to access early screening [14]. Economically, addressing the advanced stage of colorectal cancer can be costly; for instance, chemotherapy, operation, and follow-up can cost almost $300,000 [4]. The primary purpose of our intervention is to understand why colorectal cancer rates are rising among young adults in Sioux Falls, South Dakota. By identifying the public health determinants contributing to the number of cases among young adults and organizing these factors using the socio-ecological model, we can propose an intervention to enhance prevention and early detection. Readers will learn about colorectal cancer, compare national trends to the local data available in Sioux Falls, understand the current efforts of local programs, and discover our step-by-step health plan for the future.
The Importance of a Public Health Lens
Addressing colorectal cancer through a Public Health Framework is important for several reasons. Catching the onset of colorectal cancer is beneficial, according to MD Anderson Cancer Center [29]. If the cancer is caught within the first 5 years, the survival rate is 94% for people under 50 years old [29]. With the framework, we can reduce health disparities by promoting equitable access to healthcare services such as screenings for low-income families, rural communities, and ethnic minorities. Additionally, preventing a disease is more cost-efficient than treating developed stages of cancer. We can create interventions and strategies to inform communities on proactive lifestyle choices to improve health and reduce the incidence of colorectal cancer. In summary, a public healthcare framework could prevent, detect, and lower the impact of colorectal cancer on communities.
The socio-ecological model is a framework that illustrates how multiple factors can influence a behavior. The five levels–individual, interpersonal, organizational, community, and policy–are the core concepts that are necessary for long-lasting behavior. In the case of colorectal cancer, the individual level can reveal disparities due to a lack of awareness, as well as the potential costs associated with treatment. At the interpersonal level, individuals may lack encouragement towards screenings without the support of family and friends. Healthcare providers and schools can assist at the organizational level by addressing limited healthcare access for minorities and inadequate outreach programs. On a community level, the lack of normalization around prioritizing health care and timely screenings, or even the stigma surrounding them, needs to be addressed. Finally, on a policy level, insurance coverage could pose a problem for families without insurance. Expanding these policies to provide coverage for every family would ensure an equitable environment to encourage screenings.
Methods
We took data from government and state department websites as well as reliable healthcare organizations and databases, including peer-reviewed research and testing statistics. Specifically, we obtained information from the Centers for Disease Control and Prevention (CDC), the National Cancer Institute (NCI), and the South Dakota Department of Health. We also extracted data from institutional websites such as Sanford Health, GetScreenedSD, Live Well Sioux Falls, and Avera Health. Additionally, PubMed and Google Scholar were consulted to identify national trends, research related to colorectal cancer risk factors, and the impact of social determinants of health. We also consulted data and updated screening recommendations from the American Cancer Society.
We conducted a literature review to provide more recent context reflecting the most updated trends and risk factors for the Sioux Falls population. We also focused specifically on colorectal cancer screening access, social and biological aspects behind disparities in outcomes, and trends among younger populations ages 20-45 [18]. We also prioritized credible health organizations because of their reliability and current recommendations on screening guidelines. We did not include articles that were outdated or irrelevant to our specific area of study. Studies that only focused on advanced treatment technologies were used less often because our primary purpose was to understand prevention and community-level interventions. In total, we reviewed 25 articles for this paper.
Our stakeholders came from a variety of different backgrounds and perspectives surrounding colorectal cancer. These stakeholders were important based on their personal history in Sioux Falls and their diagnosis with colorectal cancer at some point in their lives. We selected patients diagnosed at various stages of their lives to create a more diverse group of stakeholders. Our first stakeholder helped us specifically with the medical side of colorectal cancer. Our next stakeholder was an oncology nurse who had several years of experience caring for patients with colorectal cancer and chemotherapy in addition to her diagnosis with the cancer. Our final interview was conducted with a Sioux Falls resident who was recently diagnosed with colorectal cancer, from whom we gained insight into the diagnostic process. We compared our interviews with each of these stakeholders to determine the importance of our topic and how exactly to approach our final 12-month plan.
We designed our plan of action by primarily determining the concerns and conditions surrounding colorectal cancer. With the information provided by our stakeholders in Sioux Falls, we identified a knowledge gap regarding the personal risks associated with their lifestyle habits and genetics. Of the several patients we interviewed, a major concern was the 10-year interval between each screening. The stakeholders discussed how the cancer could spread rapidly within a short time and thus the importance of early action. With this insight, we focused our plan of action on early detection, educating the community, and providing equitable care for isolated populations.
National Literature Review
According to The Colorectal Cancer Alliance, “[i]n 2025, colorectal cancer is the fourth most commonly diagnosed cancer and the second leading cause of cancer deaths in the United States,” with an estimated 154,270 new cases and 52,900 deaths expected in 2025 [10]. Since the early 2000s, the prevalence of colorectal cancer in people under the age of 50 has continued to rise about 2.4% each year [23]. Some groups are at a higher risk for developing colorectal cancer. For instance, men are more often diagnosed than women are, and African Americans are around 20% more likely to be diagnosed and 40% more likely to die from the disease in comparison to White Americans [2]. Alaska Natives and American Indians also have high rates of incidence and mortality [19]. These discrepancies result from factors such as socioeconomic challenges, access to healthcare, and environmental influences. Obesity, alcohol and tobacco use, poor diet and malnutrition, and physical inactivity also contribute to the rise of colorectal cancer [17].
People of lower socioeconomic status can face financial difficulties that prevent them from accessing regular screenings or treatment. Without a stable job or insurance, colonoscopies are expensive, even when medically necessary. Individuals with low health literacy may be unaware of the warning signs and therefore may not get screened. Limited access to healthcare may also prevent screenings and colonoscopies, which are essential for detecting colorectal cancer before it spreads. Neighborhood and environmental factors can also affect individuals’ health choices, including food availability, opportunities for exercise, and safety. Underserved or low-income communities are at increased risks for colorectal cancer as a result of unhealthy diet, physical inactivity, or lack of medical appointment availability. Lastly, mistrust in the healthcare system, stigma, and lack of culturally sensitive care can all influence an individual’s use of preventive services.
Justification for Target Population
Our research team, composed of members from Illinois, South Dakota, and Texas, has reported the most disproportionate findings from Sioux Falls, South Dakota. With 9.64% of the population considered low-income and living in poverty, this community is at high risk of being diagnosed with colorectal cancer [16]. Colorectal cancer is one of the leading causes of cancer-related deaths in Sioux Falls. From 2016 to 2020, South Dakota saw an average of 398 newly invasive colorectal cancer cases per year, making up about 9.0% of all cancer deaths [14]. The rise of colorectal cancer is meaningful because many individuals under 45 are not routinely screened for it [26]. Raising awareness among young adults and healthcare providers is crucial for detecting early symptoms and preventing delays in diagnosis.
Individual: Lifestyle choices can make a significant impact on physical and individual health. Diets high in fiber, fruits, vegetables, and whole grains can reduce the risk for colorectal cancer. Conversely, consuming red or processed meat and high alcohol intake are dietary habits that increase the risk for colorectal cancer [28]. Besides diet, genetics can play a role in the development of colorectal cancer. Inherited gene mutations, such as Lynch Syndrome and Familial Adenomatous Polyposis, can increase an individual’s chances of being diagnosed with colorectal cancer. With these factors in mind, we must promote a healthy and active lifestyle for the community of Sioux Falls.
Interpersonal: Family support, peer relationships, and social networks play a crucial role in determining how individuals manage their health. Patients with a sound support system are more likely to attend screenings, follow treatment guidelines, and experience better mental or physical outcomes as a result. On the other hand, those facing social isolation have higher risks of delayed care and, in turn, poorer quality of health. With the increase in cases of colorectal cancer among younger individuals, building a strong network as a foundation and having familial support in Sioux Falls is essential to improving the proper management of this disease.
Organizational: The steps we can take on an organizational level include community-based initiatives that focus on patient accessibility and enhance treatment opportunities. Sanford Health from 2015-2019 increased the number of screenings through colonoscopies or standardized screenings by 78.1% according to the American Cancer Society National Colorectal Cancer Roundtable [22]. Encouraged screenings in workplace and community settings can make prevention and early detection of colorectal cancer more accessible to a larger group of people. These organizational measures in Sioux Falls can ensure a patient’s best chance at recovery.
Community: Major hospitals in this area, such as Sanford Health or Avera Health Center, provide local care and education regarding this cancer. They provide articles on how to prevent colorectal cancer, what colorectal cancer is, and what treatments might look like [5]. At the Avera Cancer Institute, several clinical trials are in place to improve the quality and options of treatments for these patients [6]. In addition, South Dakota State University and the University of South Dakota have published research exploring the role of age and gender in colorectal cancer [13]. Overall, Sioux Falls offers resources to improve the lives of those diagnosed with colorectal cancer.
Policy: The South Dakota Department of Health provides general information about colorectal cancer, various screening options, and risk factors for developing the disease. According to GetScreenedSD, 75.3% of people from South Dakota were screened for colorectal cancer in 2020 [14]. The state-level programs encourage safety and ultimately decrease the incidence of colorectal cancer in the state. Furthermore, 72% of people in South Dakota are classified as overweight [25]. Because obesity is a leading risk factor for colorectal cancer, the state may need to implement interventions to lower the impact of this high prevalence. Other risk factors, including smoking and alcohol use, are also linked to colorectal cancer.
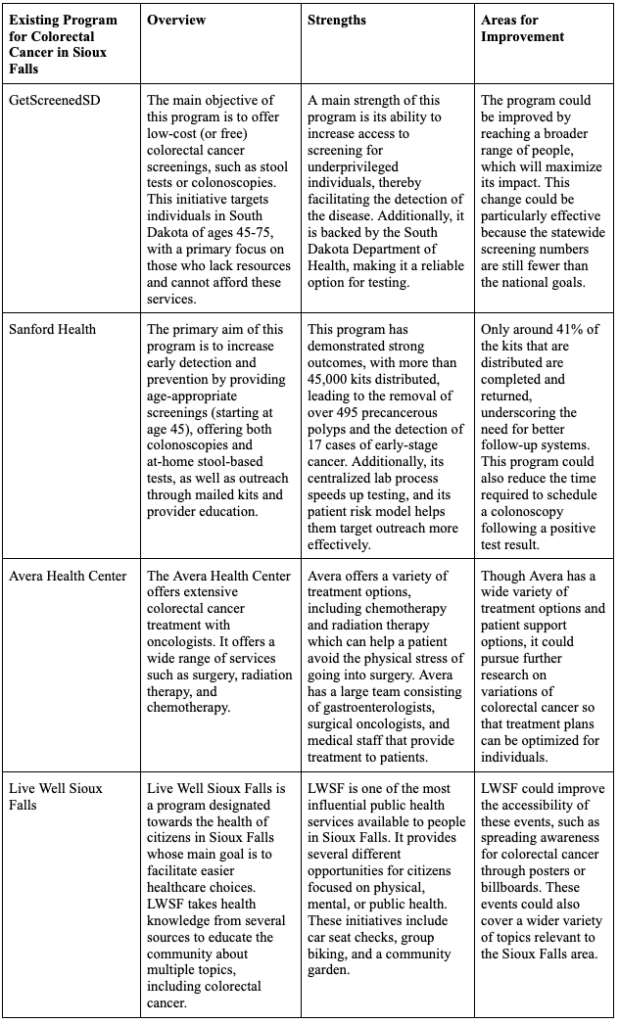
Table 1: Overview of Colorectal Cancer Programs for Individuals Aged 20-45 in Sioux Falls
Stakeholder Perspectives
We interviewed three stakeholders: Dr. Ashish Atreja, MD, MPH; Katy Billion; and Patti Vandenburg. Dr. Atreja is a gastroenterologist and public health expert from New York. He addressed colorectal cancer by highlighting its importance and the lack of awareness within the community. Katy Billion is a local oncology nurse, sharing both patient and provider perspectives. She offered us insight into why colonoscopies are important, the process of treatment, and how colonoscopy schedules change after being diagnosed with this cancer. She noted parallels with younger relatives’ cases and national trends. She supported lowering the screening age or shortening the interval time, and indicated that alternative solutions to colonoscopies are challenging to identify. Patti Vandenburg, our final stakeholder, provided the perspective of an individual who was recently diagnosed with colorectal cancer and expressed a desire for increased research on the disease.
Digital Health Solutions
The Quintuple Aim model is a process devoted to health equity in order to improve healthcare and promote value-based care. This model is a framework for addressing colorectal cancer because it ensures that Sioux Falls can reduce case incidence, improve care, and eliminate disparities in treatment between populations. With this model, the shift toward digital solutions has increased the availability of health data. Digital health solutions include telehealth services and applications that are expanding access to healthcare, reducing costs by minimizing unnecessary hospital visits by providing alternate, virtual care. Overall, these technological advances are promoting health equity and improving treatment rates in underserved populations.
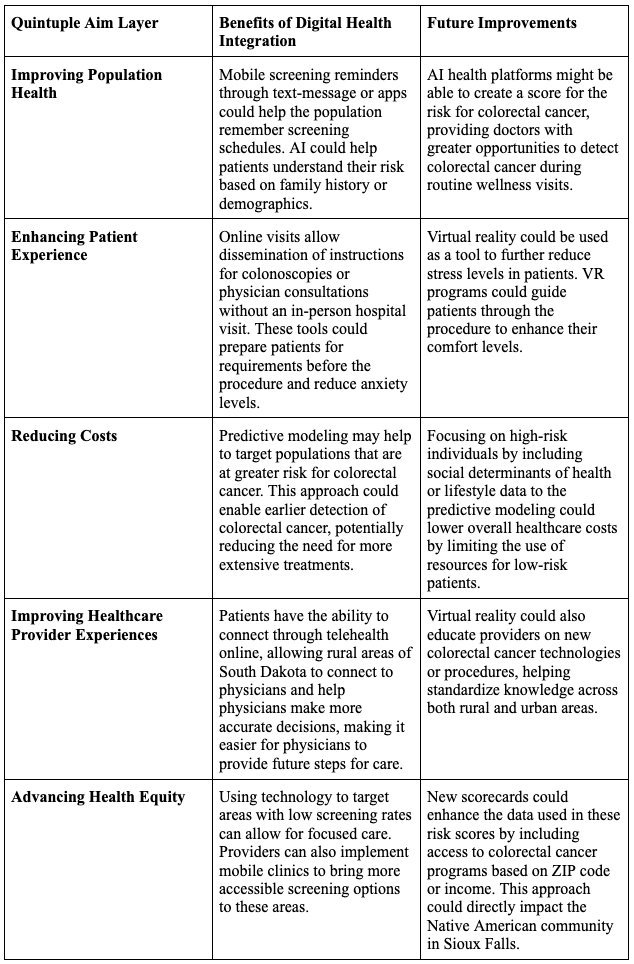
Table 2: Quintuple Aim Model for Colorectal Cancer in Young Individuals
Plan of Action
Our plan of action includes a twelve-month intervention program focused on the early detection and prevention of colorectal cancer among young adults ages 20-45 in Sioux Falls. We will divide our plan into three phases. With this intervention, our goal is to educate the high-risk population about colorectal cancer, reinforce prevention, and promote healthy behaviors.
In August through November, phase one will focus on identifying screening patterns, mortality rates, and any barriers encountered during our intervention. To raise awareness, we will distribute educational materials and host community events. At the same time, we will compile data and design communications for the importance of a healthy diet, early screenings, and an active lifestyle. Additionally, we will hold assemblies with oncologists and local leaders to target our high-risk population. When launching our awareness campaign, our focus will revolve around identifying warning signs of colorectal cancer and the steps to take once the symptoms are recognized. With this first phase and the help of local federal and state organizations, we hope to reduce the risk for early colorectal cancer in Sioux Falls.
During our second phase, which spans from December to March, our goal is to educate those who are at high risk for colorectal cancer. Specifically, we want to spread awareness on how this cancer develops and the preventative measures that can be taken against the rise of colorectal cancer. Providing equitable care for Sioux Falls is essential for prevention and early detection. We will partner with healthcare facilities and gyms to promote screenings and health assessments, and begin advocating for earlier screening recommendations throughout the community. We will also implement workshops, workplace wellness programs, and patient advocacy. In addition, collaborating with dietitians, fitness centers, and healthcare providers will provide risk-reducing guidance and evidence-based information. We will carry out initiatives that will include social media infographics on local health facility websites and popular locations during Colorectal Awareness Month. Furthermore, we will send out mobile screening events, such as low-cost fecal immunochemical tests, to underserved communities lacking healthcare resources, providing cost-effective care. Additionally, providing pop-up colonoscopy screenings in rural areas monthly can provide immediate access to early detection of colorectal cancer.
From April to July, our third and final phase will be to evaluate and review implementation progress. When considering our intervention program, we can address any disparities and provide accessible care while advocating for policy change. With an alarming number of early-onset colorectal cancer diagnoses, we must adjust the current policy. Encouraging colonoscopies for the target population could institutionalize our intervention and confirm that it is sustainable, impactful, and long-term. With increased funding and collaborations, we would continue to expand our intervention program to nearby suburbs in Sioux Falls to continue the spread of equitable care to those who are isolated or unaware of the risks for developing early-onset colorectal cancer.
During our intervention, we will implement our plan in three steps: educating through various media channels, raising awareness through collaborative events, and launching a targeted social media campaign. We plan to distribute campaign materials to coffee shops, bookstores, billboards and gyms because of widespread access by younger individuals. We could partner with Avera for a cancer awareness event to educate more individuals about colorectal cancer. However, it is possible that we may be unable to access larger platforms such as billboards, or be permitted to post materials publicly; in such cases, we can instead use online infographics on social media. Additionally, if individuals are unable to collaborate with us specifically on colorectal cancer, we could host our event, virtual or in person, to bring attention to this important topic and raise awareness.
Discussion
We have noticed an alarming increase in the rate of colorectal cancer diagnoses in younger adults between the ages of 20-45 in Sioux Falls. Sioux Falls healthcare facilities, Avera and Sanford, advocate the importance of screenings, especially colonoscopies, as an effective way to detect colorectal cancer. Additionally, only 38% of stores in Sioux Falls located in food deserts have fresh fruit available [27]. A well balanced diet and active lifestyle is crucial to health and bodily systems, thus also influencing colorectal cancer development. Taking these barriers on at a multidisciplinary approach can ensure a plan that focuses on equitable treatment, prevention, and healthcare access across rural and urban areas of Sioux Falls.
Early-stage diagnosis can reduce treatment costs and alleviate financial burdens on low-income families. In the workplace, digital tools to encourage self-regulation of vitals in patients could ease the cognitive burden of physicians. These digital tools could be in the form of a wearable or a mobile app that keeps track of a patient’s daily activity. If a patient actively monitors their habits and receives direct warnings based on their habits, they may be more likely to become aware of the consequences of not seeking preventative treatment. Continuous evaluation of our intervention is important to ensuring that there are no disparities or gaps that could prevent individuals from seeking treatment.
Conclusion
Colorectal cancer remains a significant public health concern both nationally and locally. It is the third most prevalent cancer, with more than 154,000 new cases and nearly 53,000 deaths expected in 2025, and Sioux Falls is not free from these statistics [3]. The increasing rate of diagnoses in younger adults, particularly those under 45, requires an immediate and targeted approach to prevention. Our plan focuses on reaching younger populations through relatable, community-based outreach and efforts to spread awareness in locations where younger people commonly visit. In the future, we envision this project expanding beyond Sioux Falls. We aim to normalize early screening and preventative health education in communities nationwide. Future research should further explore how digital tools, personalized risk estimates, and culturally tailored outreach may help close the screening gap.
References
- Ahnen, Wade, Jones, Sifri, Silveiras, & Greenamyer, et al. (2014). The Increasing Incidence of Young-Onset Colorectal Cancer: A Call to Action Author links open overlay panel. Elsevier, Vol. 89 (Iss. 2), 216-224. https://www.sciencedirect.com/science/article/abs/pii/S0025619613008227
- American Cancer Society. (2020, September 3). Colorectal cancer rates higher in African Americans, rising in younger people. American Cancer Society. Retrieved January 10, 2026, from https://www.cancer.org/cancer/latest-news/colorectal-cancer-rates-higher-in-african-americans-rising-in-younger-people.html
- American Cancer Society National Colorectal Cancer Roundtable. (2025, August 5). Data and progress. Retrieved January 10, 2026, from https://nccrt.org/our-impact/data-and-progress/
- Bhimani, N., Wong, G. Y. M., Molloy, C., Pavlakis, N., Diakos, C. I., Clarke, S. J., Dieng, M., & Hugh, T. J. (2022). Cost of treating metastatic colorectal cancer: A systematic review. Public Health, 211, 97–104. https://doi.org/10.1016/j.puhe.2022.06.022
- Cancer Coalition, S. D. (2020, April). South Dakota Cancer Coalition. Cancer Incidence and Mortality Among South Dakotans, 2017. Retrieved August 1, 2025, from https://www.cancersd.com/about-cancer/#:~:text=Lung%20and%20bronchus%20cancers%20were,SEER%202017%20rate%20of%20152.6.
- Colon and rectal cancer. (n.d.). Avera. Retrieved July 30, 2025, from https://www.avera.org/services/cancer-care/cancer-types/colon-rectal-cancer/
- Colon cancer facts. (2025, March 18). Colon Cancer Coalition. Retrieved July 30, 2025, from https://coloncancercoalition.org/colon-cancer-screening/facts/
- Colorectal cancer. (2025, February 26). Centers for Disease Control and Prevention. Retrieved July 30, 2025, from https://www.cdc.gov/colorectal-cancer/index.html
- Colorectal cancer. (2025). Live Well Sioux Falls. Retrieved July 30, 2025, from https://livewellsiouxfalls.org/feel-well/physical-health/cancer/colorectal-cancer/
- Colorectal cancer facts and statistics. (2025). Colorectal Cancer Alliance. Retrieved July, 30 2025, from https://colorectalcancer.org/basics/facts-and-statistics
- Colorectal cancer information: Understanding colorectal cancer. (2024, March 19). American Cancer Society. Retrieved July 30, 2025, from https://www.cancer.org/cancer/types/colon-rectal-cancer.html
- Colorectal cancer screening. (n.d.). Sanford Health. Retrieved July 30, 2025, from https://www.sanfordhealth.org/medical-services/cancer/cancer-screenings/colorectal-cancer-screening
- Community health status report. (2025). Sioux Falls Government. Retrieved July 30, 2025, from https://www.siouxfalls.gov/files/assets/public/v/1/health/public-health/community-health-status-report-2025.pdf
- Department of Health, S. D. (2025). Colorectal Cancer Control Program. GetScreenedSD. https://www.getscreenedsd.org/colorectal-cancer-program
- Garry, M. (2025, February 11). Sanford mails colon cancer test kits to 45,000 patients. Sanford Health News. Retrieved July 30, 2025, from https://news.sanfordhealth.org/healthy-living/sanford-mails-colon-cancer-test-kits/
- Kitzman, M. (n.d.). Sioux Falls, SD. Data USA. Retrieved August 1, 2025, from https://datausa.io/profile/geo/sioux-falls-sd/
- National Cancer Institute. (2020, July 6). Colorectal cancer rising in younger adults. National Cancer Institute. Retrieved January 10, 2026, from https://www.cancer.gov/news-events/cancer-currents-blog/2020/colorectal-cancer-rising-younger-adults
- New ACS study shows cancer mortality rates among black people declining, but remain higher than other racial and ethnic groups. (2025, February 20). American Cancer Society. Retrieved July 30, 2025, from https://pressroom.cancer.org/CancerStatisticsforAfricanAmericanandBlackPeople
- Office of Minority Health. (n.d.). Cancer and American Indians/Alaska Natives. U.S. Department of Health and Human Services. Retrieved January 10, 2026, from https://minorityhealth.hhs.gov/cancer-and-american-indiansalaska-natives
- Park, S., & Myers, M. (2024, October 9). SD Cancer Coalition 2024 Fall Meeting. SD Cancer Coalition. Retrieved 1 August, 2025, from https://www.cancersd.com/wp-content/uploads/2024/10/Fall-Meeting-Slides-2024.pdf
- Press releases. (2023, March 1). American Cancer Society Press Room. Retrieved July 30, 2025, from https://pressroom.cancer.org/CRCFactsFigures2023
- Ross, T. (2019, August 29). Interview with Sanford Health—80% By 2018 National Achievement Award Honoree. National Colorectal Cancer Roundtable. Retrieved August 1, 2025, from https://nccrt.org/interview-with-sanford-health-80-by-2018-national-achievement-award-honoree/
- Siegel, R. L., Wagle, N. S., Cercek, A., Smith, R. A., & Jemal, A. (2023). Colorectal cancer statistics, 2023. CA: A Cancer Journal for Clinicians, 73(3), 233–254. https://doi.org/10.3322/caac.21772
- South Dakota cancer screening program. (2025). GetScreenedSD. Retrieved July 30, 2025, from https://www.getscreenedsd.org/hubfs/2023CRCmonographpdf.pdf?hsLang=en
- South Dakota Department of Health. (2020). Overweight and obese: Behavioral Risk Factor Surveillance System 2020. Retrieved January 10, 2026, from https://doh.sd.gov/media/zbphxvoz/brfss-2020_overweightobese.pdf
- Stoffel, E. M., & Murphy, C. C. (2021, January). Epidemiology and mechanisms of the increasing incidence of colon and rectal cancers in young adults. Gastroenterology. Retrieved July 30, 2025, from https://pmc.ncbi.nlm.nih.gov/articles/PMC6957715/
- Suzanne, Arega, Bishop, Chime, Dolma, Teller. Food security & food access in Sioux Falls, SD. (2022, May). Augustana Research Institute for Sioux Falls Thrive. Retrieved July 30, 2025, from https://www.augie.edu/sites/default/files/documents/2022-06/Thrive%20Food%20Security%20Report%20Update%202022%20final.pdf
- Vallis, J., & Wang, P. (2022, June 27). The role of diet and lifestyle in colorectal cancer incidence and survival. National Library of Medicine. Retrieved July 28, 2025, from https://www.ncbi.nlm.nih.gov/books/NBK585999/
- You, N. (2024, July 9). Why are young adults getting colorectal cancer? MD Anderson Cancer Center. Retrieved July 30, 2025, from https://www.mdanderson.org/cancerwise/why-are-more-young-adults-getting-colorectal-cancer-what-to-know.h00-159385890.html
Related Posts
Medical Overtreatment in the United States: Causes, Consequences, and Solutions
This article was originally submitted to the Modern MD competition...
Read MoreThe E.C.H.O. Initiative: Encouraging Cardiovascular Health Through Outreach
This publication is in proud partnership with Project UNITY’s Catalyst Academy 2023...
Read MoreTrust: The Essence of Good Policy Implementation
Figure 1 President Tsai Ing-wen inspects the Central Epidemic Command...
Read MoreThermophilic Life in Yellowstone National Park Challenges the Physical and Chemical Limits of Survival
Cover Image: Grand Prismatic Spring in Yellowstone National Park (Source:...
Read MoreThe Influence of Language on the Perception of the World
Figure 1: The Influence of Language on the Perception of...
Read MoreDarius Dastur, Mishal Ali, Harshitha Ezhilarasan, Hasan Khan, Aaron Akasala