This publication is produced in partnership with Project UNITY’s Catalyst Academy Class of 2025, a student public health research and education program.
Abstract
Alzheimer’s disease is a neurodegenerative condition characterized by progressive memory loss and cognitive impairment. While typically a medical diagnosis, Alzheimer’s disease also presents significant public health implications. This report aims to investigate both national and local prevalence of Alzheimer’s disease and dementia, and aims to explain how public health determinants can inform the development of a community-focused prevention in Baltimore. This report further aims to define how public health principles can be utilized to improve the quality of life for adults at risk for Alzheimer’s disease and dementia. A literature review was conducted using PubMed, JAMA network, and the National Institute of Health. A total of 39 peer-reviewed articles were reviewed and selected based on their credibility and relevance to the issue. Findings indicate that older adults, particularly Hispanic and Black populations in Baltimore, Maryland, are at higher risk for Alzheimer’s disease and related dementias compared to other racial and ethnic groups. Social determinants of health, including access to healthcare and economic stability, also influence risk, as limited income may contribute to risk factors such as an imbalanced diet, reduced physical activity, and limited access to dementia-related education. Based on these findings, a cost-effective public health prevention strategy was formulated to ensure accessibility for the target population.
Keywords: Alzheimer’s disease; dementia; Baltimore; socio-ecological model (SEM); social determinants of health
Introduction
Dementia refers to a group of neurodegenerative conditions characterized by progressive damage to neurons in the brain, leading to cognitive and motor function impairments and a reduced ability to live independently (Alzheimer’s Association, 2025). Alzheimer’s disease is the most common form of dementia. Because these conditions primarily affect people over 65, a population already considered vulnerable, targeted action is essential to support affected individuals and their families. Furthermore, the aging population in the United States continues to increase, and the number of dementia cases is expected to double by 2060 (Fang et al., 2025; Majoka & Schimming, 2021). To address this issue, organizations such as the Alzheimer’s Association provide educational programs and public resources to increase awareness of dementia risk factors and their role in the development of Alzheimer’s disease. These include non-modifiable risk factors, such as age and genetics, as well as modifiable risk factors, including poor nutrition, smoking, physical inactivity, social isolation, and limited cognitive engagement (Alzheimer’s Association, 2025). Social determinants of health, the conditions in which individuals are born, live, and work, play a critical role in shaping health outcomes and access to healthcare (Majoka & Schimming, 2021). These social determinants of health can also significantly influence the modifiable risk factors for Alzheimer’s disease and related dementia among older adults. For instance, lack of easy access to healthcare and economic instability can contribute to poor hygiene in impoverished areas, thereby increasing the overall health risk and, consequently, the risk of Alzheimer’s disease and dementia. Furthermore, risk factors such as smoking, alcohol consumption, and exposure to other chronic diseases? Diseases can cause damage to the brain that elevates the risk of these conditions.
Alzheimer’s disease and related dementia represent a major public health concern in the United States, specifically in cities and states of higher disease prevalence. With a high proportion of older adults, the city of Baltimore, Maryland, is one such region (Dhana et al., 2023). Addressing dementia in Baltimore has the potential to yield a significant positive impact on the city. With over 87,000 cases of dementia in Maryland currently, the government of Maryland has implemented initiatives aimed at reducing the prevalence of the disease. These efforts include the passage of the Dementia Services Act of 2022 and the establishment of specialized roles, such as the Director of Dementia Services Coordination (Maryland Department of Health, 2022). In addition, conducting comprehensive research and developing solutions in Baltimore can drive meaningful change at the grassroots level.
Public Health Lens
Alzheimer’s disease and dementia must be addressed through a public health framework as their growing prevalence indicates that addressing the issue at the individual level is insufficient. A public health approach is better for addressing this widespread issue because it emphasizes community health, overall well-being, and preventative measures. Given that Alzheimer’s disease currently has no cure, disease prevention remains the most effective means of reducing the number of individuals affected by this disease.Although certain drugs may slow disease progression, the primary focus still remains on lowering risk (Alzheimer’s Association, 2025).
A public health framework would also consider various non-medical factors, commonly referred to as social determinants of health (SDOH), which significantly contribute to disease risk. The five primary categories of SDOH include economic stability, education, social and community context, health and healthcare access, and neighborhood and built environment (US Department of Health and Human Services, 2020). These determinants are particularly relevant to Alzheimer’s, as it is considered a non-communicable disease. An approach integrating SDOH enables the development of more effective and sustainable interventions, working to reduce dementia prevalence.
The socio-ecological model (SEM) further enhances understanding of Alzheimer’s and dementia risk as this illustrates how factors across multiple levels (individual, interpersonal, institutional, community, and policy) interact to influence health outcomes (Golden & Earp, 2012). For example, diet is a key factor that influences risk of Alzheimer’s at the individual level (Alzheimer’s Association, 2025). While the Mediterranean diet is associated with reduced risk of Alzheimer’s and related dementia, diets high in fat, sodium, and cholesterol content are linked to increased risk. At the interpersonal level, social interaction is highly relevant, as active interactions with others have been shown to lower dementia risk (Alzheimer’s Association, 2025). At the organizational level, education initiatives at schools and workplaces—ranging from academic learning to fitness programs—can contribute to risk reduction. Community-level interventions, including awareness campaigns, are highly beneficial because increased awareness can promote healthy habits and the modification of risk factors. Finally, at the policy level, state legislation in Maryland has demonstrated a commitment to addressing Alzheimer’s disease and related dementia through laws. (Maryland Department of Health, 2022).
Methodology
A literature review of 38 articles was conducted. Articles were sourced from scholarly databases, including PubMed, PubMed Central, and the ProQuest platform, as well as peer-reviewed journals such as the Journal of the American College of Cardiology (JACC). Additional sources included government databases—such as the Centers for Disease Control and Prevention (CDC), the Food and Drug Administration (FDA), and San Diego County government resources—and reputable organizations including Million Hearts, Live Well San Diego, and Statista Atlas.
To gain more in-depth, professional opinions, twenty-one stakeholders were contacted across different organizations and specialties related to CVD in San Diego. Of those stakeholders, three expressed interest in collaborating in an online meeting, conducted via Zoom, to further discuss their perspectives on the issue. Ultimately, the information gathered has enabled our team to synthesize several proposed solutions for reducing CVD prevalence among San Diego Chicanx/Latinx elderly.
Literature Review
CVD is a growing public health concern in the United States, consistently standing as the leading cause of mortality in the U.S., as affirmed by the Centers for Disease Control and Prevention, causing 702,880 deaths in America in 2022 (CDC, 2024). Over eight million Californians are living with at least one of the most common forms of cardiovascular disease, which are heart disease, heart failure, stroke, or high blood pressure, which is a major risk factor for heart disease and stroke. (Hispanic Heart Health, 2024).
Among these statistics, Hispanics are to be especially vulnerable as compared to non-Hispanic whites: even more so when considering how Hispanics are often more vulnerable both in SDOHs and CVD risk factors like chronic conditions such as diabetes, hypertension, and obesity (Balfour et al., 2016; Rodgers et al., 2019). 1 in 6 Chicanx with CVDs live in poverty in the U.S., limiting their access to healthcare and exacerbating CVD outcomes (Bohn et al., 2019). Sociocultural factors such as poor health literacy, language barriers, and differing perspectives on Western medicine may delay key medical interventions.
Justification for the Target Population
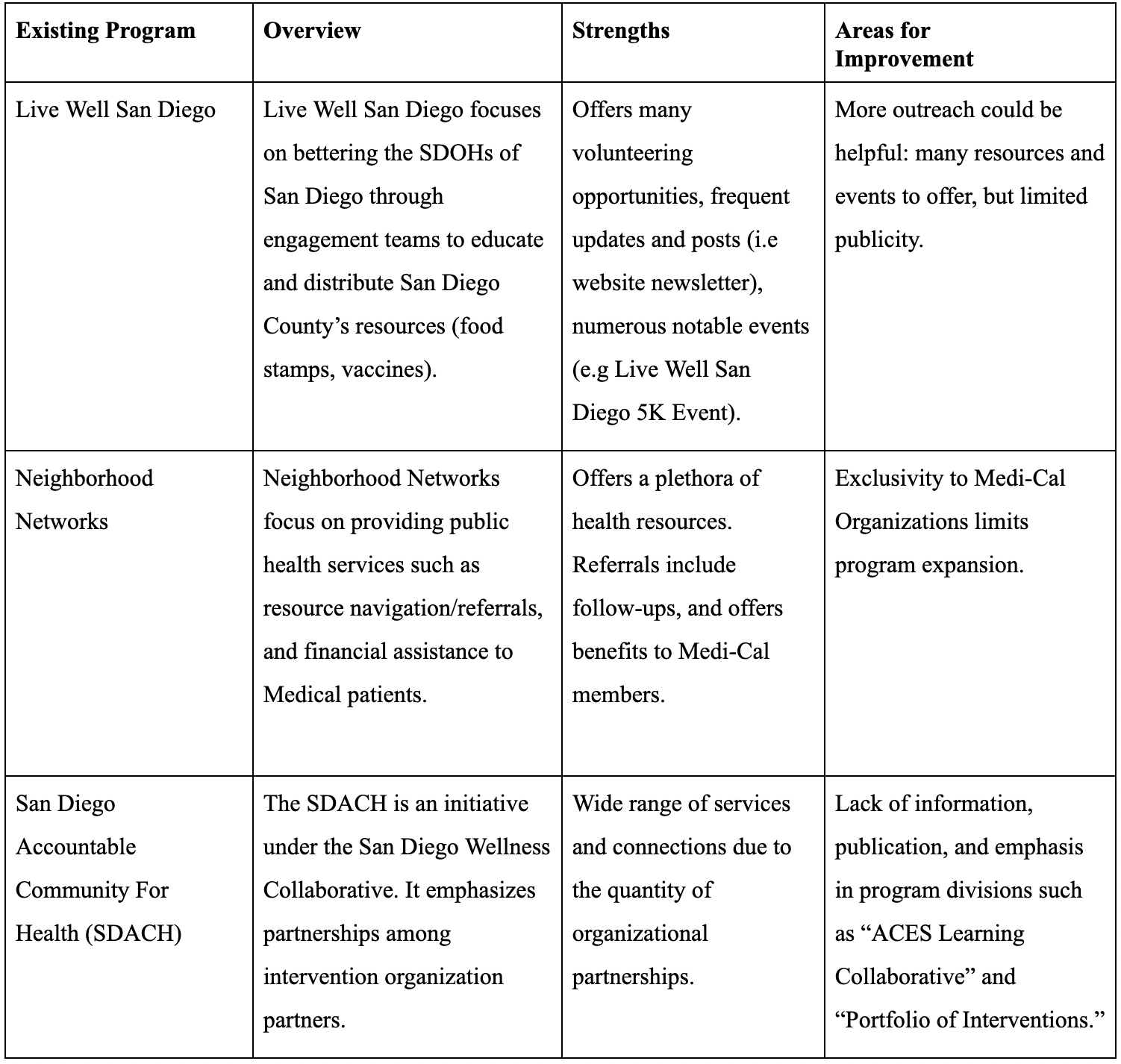
Table 1: Existing San Diego CVD Reduction Programs
Stakeholder Perspectives
The insights and observations of all three of our interviewed stakeholders confirm the findings of our literature review: that the American Chicanx population faces greater challenges related to SDOHs and CVD risk factors in areas like San Diego, as well as the significance of cultural and language barriers. Another common emphasis among all three professionals, which we had not previously considered, was the importance of implementing culturally appropriate public health strategies. Both the representative of the Institute of Chicanx Psychology and Professor Rosanna Alvarez of Chicana & Chicano Studies agreed that many aspects of traditional Chicanx culture are healthy, including their tradition of family activities and cuisine. Therefore, all suggested that an intervention focusing on this population should implement existing qualities of traditional Chicanx culture.
Digital Health Solutions
To address the need for improvement in equitable access to healthcare, the Quintuple Aim builds on the Triple and Quadruple Aim (Gould, 2022) to emphasize inclusion and serving the population. The Quintuple Model consists of five main objectives. Improving population health, enhancing the patient experience, reducing costs, improving healthcare providers’ experiences, and advancing health equity (Interwell Health, 2024). We apply the Quintuple Model to understand how digital health tools, such as remote patient monitoring and telehealth— which increase remote accessibility and cost efficiency—can manage chronic conditions like cardiovascular disease (Martin R Cowie et al., 2021; Kuan et al., 2022; Sarah Raes et al., 2024).
The current technical shift towards the digital transformation of health care systems has experienced a clear shift in the last few years, leading to improvements in cardiovascular patient care, accessibility, and cost reduction (Breitschwerdt, R. 2023). Digital solutions can also address health illiteracy and language, and access to proper transportation to visit a physician in person.
Chronic diseases such as heart failure have a huge health economic importance because of their high mortality. Telemedicine offers a unique opportunity to replace crucial in-person visits, such as with the use of wearable technology, mobile apps, and telemedicine (Stremmel, C., & Breitschwerdt, R., 2023). These digital tools can improve individual engagement and adherence through accessible personalized instructions, real-time monitoring, and remote consultations, making it easier to manage and access their cardiovascular health (Wu. A et al., 2025).
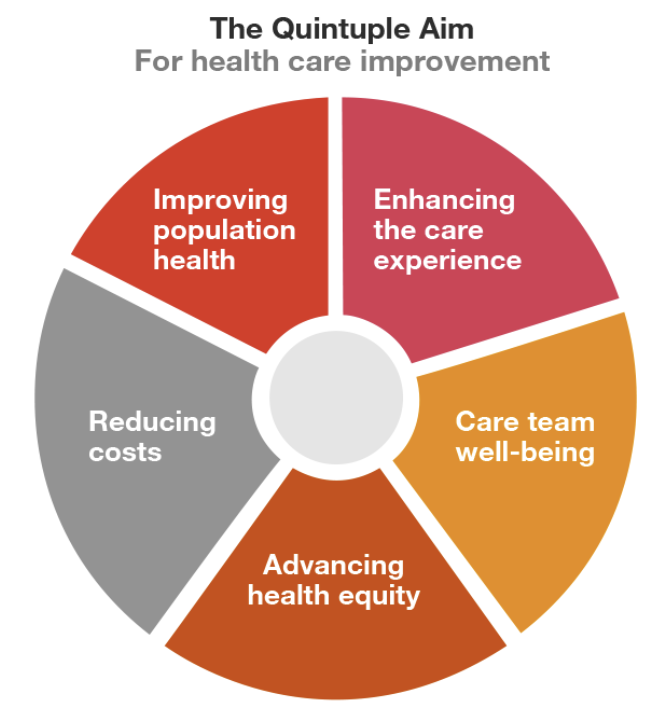
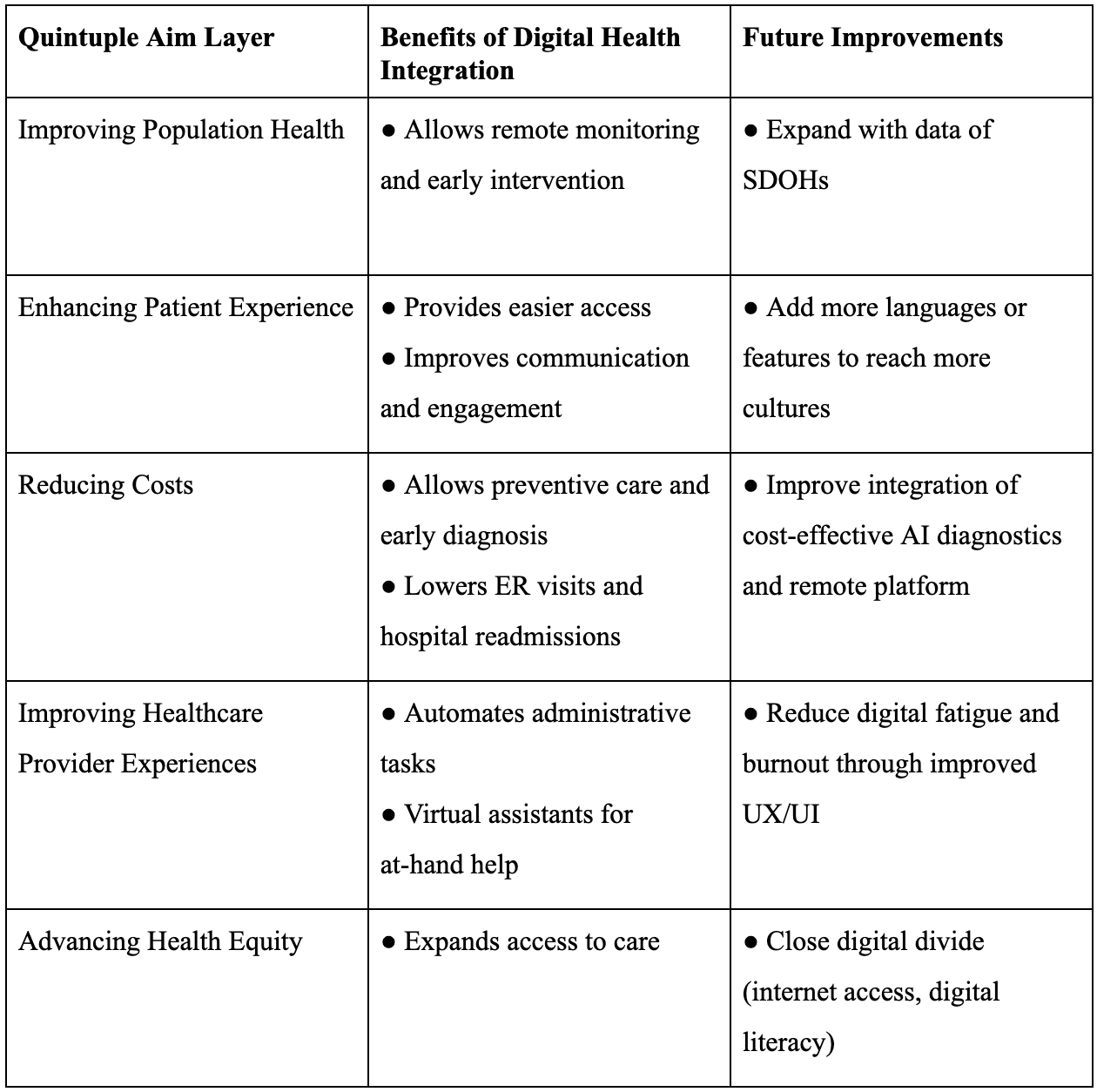
Table 2: Quintuple Aim of Healthcare
Plan of Action
The intervention’s main objective is to encourage and ultimately increase the adoption of healthier lifestyles among elderly Chicanx San Diego residents aged 50 or older; however, our strategy’s applicability is not necessarily limited to San Diego or Chicanx people. We aim to address CVD risk by focusing on three major lifestyle factors that contribute to CVD risk: adequate and proper physical activity, a balanced diet, and substance use. Our plan is centered around a 4-month motivational-interviewing program, a program that consists of weekly health meetings—offered virtually and in-person to increase accessibility—between health professionals and clients to monitor and motivate clients on their path towards self-improvement, which may include nutritional, exercise, or substance or alcohol reduction practices. These weekly meetings aim to motivate clients in their lifestyle changes and effectively maintain their accountability on their health improvement journey and sustainability.
This intervention will take place from January to March, with a period of fundraising that includes searching for project grants, local and federal government assistance, local business collaborations, and individual donations (both online and in-person). We will also address our need for venues and suitable meeting locations by reaching out to managers of suitable locations (such as vacant classrooms, community centers, etc.), saving operating costs and making effective use of available resources. The funds we collect during this period will be used to purchase equipment for venues and provide salaries for the participating healthcare professionals.
With sufficient collected funding, we will seek out health counselors and professionals from sources and institutions such as the Institution of Chicanx Psychology & Community Wellness from April through May to secure both in-person and online counseling services for our program.
June will consist of committee and health professional meetings to facilitate cohesion and clarity in tasks and standards for client meetings and venue management. In the same month, we will conduct a period of vigorous publicity and advertising using several methods, such as booths and representatives in public spaces ( including markets, parks, and public events), social media, and physical flyers, brochures.
By July, we will officially open our services and begin our counseling sessions, which will run until the end of October. This will include a large orientation for all participants to launch the program. Throughout these months, we will hold weekly to biweekly meetings with all counselors to evaluate progress, strengths, and difficulties faced, and work towards improving at every meeting.
Once the four-month intervention period is over, we will survey our clients through interviews and questionnaires, as well as assess their improvement in the three areas of cardiovascular health: physical activity, diet, and substance abuse. With feedback from clients, we will conduct a two-month evaluation period with all counselors and the intervention committee to analyze the effectiveness of the intervention.
Project UNITY was the program that first galvanized the formation of our research team and intervention, and it can continue to offer guidance and counseling to our team. Moreover, Project UNITY can continue to aid in the outreach to stakeholders, collecting valuable and professional insights and data. Finally, Project UNITY could be an excellent source for publication, advertising, and overall public outreach for intervention efforts.
Strengths and Limitations
One of the program’s biggest strengths is accessibility both in person and online with weekly virtual meetings with professionals working in the health industry. For this approach, we will also be making it cost-free in order to cater to low-income families who have trouble accessing the proper medicare. A limitation may be the resource-intensive nature of the program, which includes devices and bilingual professional staff. Additionally, our program indirectly helps the population, and systemic factors such as our program indirectly helps the population and systemic factors such as air pollution will remain, which plays a major factor in CVD.
Discussion
San Diego’s elderly Chicanx often are disadvantaged in both Social Determinants of Health (SDOH), (including housing stability and quality of life) as well as risk factors associated with aging. We took a community-centered effort and a multidisciplinary approach using the Quintuple Aim Model and digital health to reduce CVD risk by taking a unique approach to engaging clients. Our intervention was a motivational interviewing-based program , in which CVD health counselors tracked clients’ behaviors in three key focus areas— diet, physical activity, and substance use behaviors. The clients have weekly virtual meetings over four months to help facilitate accountability and promote behavior change.
We envision the Quintuple Aim to improve the healthcare worker experience by reducing burnout through enabling remote participation and potentially allowing for fair payment or commission based on fundraised amounts. In addition, as we continue to aim for health equity and cost savings, we have structured the program to be free of charge to participants. Moreover, our funds will allow us to equip clients with free digital devices that are necessary for remote sessions, which eliminates the possible technology-related barriers related to care.
To strengthen the sustainability and adaptability of this intervention, we will conduct annual evaluations with the participants, counselors, and committee members. These meetings will facilitate constructive feedback, and articulate possible improvements to the intervention next time. We believe that through any cultural responsiveness, we will provide the means necessary to uniquely address and significantly reduce the CVD risks of the older Chicanx segment of the population living in San Diego.
Conclusion
As affirmed by both our scoping literature review and interviews with several relevant professionals, CVD is a significant health issue amongst Elderly Chicanx over the age of 40 in San Diego. They are one of the highest ethnic groups to be prone to the disease. Thousands of Hispanics suffer from at least one CVD risk factor. Those in unprivileged communities often struggle with financial problems, language barriers, and limited access to healthcare. Our intervention will be free of charge and will support the Chicanx community in San Diego to reduce CVD by restyling their daily life habits. Examples include prioritizing physical activity, hosting interactive wellness clubs, reducing substance abuse, and modifying diet. Our intervention involves hosting weekly motivational meetings both online and in person. By addressing the key factors which are the foundation to CVD development, we hope to increase our patients’ healthful autonomy and ultimately reduce its prevalence.
References
- Alba, A. D., Britigan, D. H., Lyden, E. & Johansson, P. Assessing health literacy levels of Spanish-speaking Hispanic patients in Spanish at federally qualified health centers (FQHCs) in the Midwest. J. Health Care Poor Underserved 27, 1726–1732 (2016). https://doi.org/10.1353/hpu.2016.0158
- Balfour, P. C., Ruiz, J. M., Talavera, G. A., Allison, M. A. & Rodriguez, C. J. Cardiovascular disease in Hispanics/Latinos in the United States. J. Latina/o Psychol. 4, 98–113 (2016). https://doi.org/10.1037/lat0000056
- Bohn, S., Danielson, C., Kimberlin, S., Malagon, P. & Wimer, C. Poverty in California. Public Policy Institute of California (2019).
- Calo, W. A. et al. Experiences of Latinos with limited English proficiency with patient registration systems and their interactions with clinic front office staff: an exploratory study to inform community-based translational research in North Carolina. BMC Health Serv. Res. 15, (2015). https://doi.org/10.1186/s12913-015-1235-z
- Centers for Disease Control and Prevention. Million Hearts®. (CDC, 2020).
- Centers for Disease Control and Prevention. FastStats – Heart Disease. (CDC, 2024).
- Centers for Disease Control and Prevention. Current cigarette smoking among adults in the United States. (CDC, 2024).
- Centers for Disease Control and Prevention. Heart Disease Facts. (CDC, 2024).
- Chwał, J. et al. Analysis of demographic, familial, and social determinants of smoking behavior using machine learning methods. Appl. Sci. 15, 4442 (2025). https://doi.org/10.3390/app15084442
- Cowie, M. R. & Lam, C. S. P. Remote monitoring and digital health tools in CVD management. Nat. Rev. Cardiol. 18, 457–458 (2021). https://doi.org/10.1038/s41569-021-00548-x
- Gould, K. A. Equity: Introducing the Quintuple Aim. Dimens. Crit. Care Nurs. 41, 119–120 (2022). https://doi.org/10.1097/dcc.0000000000000527
- Hardcastle, S. J. et al. Effectiveness of a motivational interviewing intervention on weight loss, physical activity and cardiovascular disease risk factors: a randomised controlled trial with a 12-month post-intervention follow-up. Int. J. Behav. Nutr. Phys. Act. 10, 40 (2013). https://doi.org/10.1186/1479-5868-10-40
- Hispanic Heart Health – Love Your Heart 2024. Live Well San Diego (2024).
- U.S. Food and Drug Administration. FDA’s Nutrition Initiatives. (FDA, 2024).
- San Diego Food Bank. Hunger Facts & Research. (2025).
- Kaplan, R. C. et al. Smoking among U.S. Hispanic/Latino adults: The Hispanic Community Health Study/Study of Latinos. Am. J. Prev. Med. 46, 496–506 (2014). https://doi.org/10.1016/j.amepre.2014.01.014
- Kuan, P. X. et al. Efficacy of telemedicine for the management of cardiovascular disease: a systematic review and meta-analysis. Lancet Digit. Health 4, e676–e691 (2022). https://doi.org/10.1016/S2589-7500(22)00124-8
- Li, Z., Xie, S. & Chen, W. The influence of the environment on adolescents’ physical exercise behavior based on family community and school micro-systems. Sci. Rep. 15, (2025). https://doi.org/10.1038/s41598-025-91387-0
- Logan Heights neighborhood in San Diego, California subdivision profile. City-Data (2025).
- Lou, P. et al. Supporting smoking cessation in chronic obstructive pulmonary disease with behavioral intervention: a randomized controlled trial. BMC Fam. Pract. 14, (2013). https://doi.org/10.1186/1471-2296-14-91
- Otto, F. When vegetables are closer in price to chips, people eat healthier, Drexel study finds. Drexel University News (2017).
- Pérez-Stable, E. J. et al. Diabetes and hypertension risk across acculturation and education levels in Hispanic/Latino adults. JAMA Health Forum 6, e250273 (2025). https://doi.org/10.1001/jamahealthforum.2025.0273
- Lavoie, J. G. et al. A family affair: Aboriginal women’s efforts to limit second-hand smoke exposure at home. (Ottawa).
- County of San Diego. REACH Program. (2018).
- Rodgers, J. L. et al. Cardiovascular risks associated with gender and aging. J. Cardiovasc. Dev. Dis. 6, 19 (2019). https://doi.org/10.3390/jcdd6020019
- Rodriguez, F. & Blumer, V. Cardiovascular health in Hispanic/Latino patients. J. Am. Coll. Cardiol. 81, 1521–1523 (2023). https://doi.org/10.1016/j.jacc.2023.02.025
- Korukonda, S. et al. Cardiovascular disease burden in the homeless population. Open Heart 12, e003190 (2025). https://doi.org/10.1136/openhrt-2025-003190
- County of San Diego Health and Human Services Agency. San Diego County Senior Health Report. (2014).
- Justice in Aging. Snapshot of Older Adults in San Diego County. (2023).
- County of San Diego. South Region Health Status Report Summary. (2023).
- Stremmel, C. & Breitschwerdt, R. Digital transformation in the diagnostics and therapy of cardiovascular diseases: comprehensive literature review. JMIR Cardio 7, e44983 (2023). https://doi.org/10.2196/44983
- University of California San Diego. Run Free Clinic Project Repeats with Gold Rating. (2025).
- United States Census Bureau. QuickFacts: California. (2024).
- Yu, E., Malik, V. S. & Hu, F. B. Cardiovascular disease prevention by diet modification. J. Am. Coll. Cardiol. 72, 914–926 (2018).
- Yu, J. et al. Associations of home-based individual and family exercise with personal and family well-being amid the COVID-19 pandemic: a population-based survey in Hong Kong. Behav. Sci. 15, 376 (2025). https://doi.org/10.3390/bs15030376
- Zarghami, F. et al. Cigarette smoking and perceived risk of cardiovascular disease in Iran. BMC Public Health 25, (2025). https://doi.org/10.1186/s12889-025-21444-w
- Zhou, X. et al. The effect of peer relationships on college students’ behavioral intentions to be physically active: the chain-mediated role of social support and exercise self-efficacy. PLoS ONE 20, e0320845 (2025). https://doi.org/10.1371/journal.pone.0320845
- Zhong, G.-C. et al. Association of ultra-processed food consumption with cardiovascular mortality in the US population: long-term results from a large prospective multicenter study. Int. J. Behav. Nutr. Phys. Act. 18, (2021). https://doi.org/10.1186/s12966-021-01081-3
Related Posts
Childhood Unpopularity May Increase Risk of Cardiovascular Disease in Adulthood
Figure 1: Childhood experiences are widely considered to affect adult...
Read MoreMedical Overtreatment in the United States: Causes, Consequences, and Solutions
This article was originally submitted to the Modern MD competition...
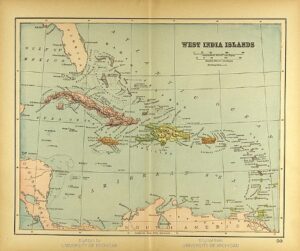
Read MoreCaribbean History through Genetics and Archaeology
Figure 1: A map of the Caribbean Islands from 1894...
Read MoreEarly Childhood Adversity Impacts Impulsive Decision-Making
Cover Image: An image of a girl holding a stuffed...
Read MoreWhen the Going gets Tough, the Close start Nearing: Networks and External Stress
Figure: A Social Network (Wikimedia Commons, Author Zigomitros Athanasios –...
Read MoreA Novel Mental Health Literacy Education Program for Pre-Teens
Figure: A typical elementary school classroom in Japan (Cassidy, 2005). Source:...
Read MoreDarius Dastur, Mishal Ali, Harshitha Ezhilarasan, Hasan Khan, Aaron Akasala